Abstract
-
Background
- Several recent studies have shown that preperitoneal pelvic packing (PPP) effectively produces hemostasis in patients with unstable pelvic fractures. However, few studies have examined the rate of surgical site infections (SSIs) in patients undergoing PPP following an unstable pelvic fracture. The purpose of the present study was to evaluate factors associated with SSI in such patients.
-
Methods
- We retrospectively reviewed the medical charts of 188 patients who developed hemorrhagic shock due to pelvic fracture between April 2012 and May 2021. Forty-four patients were enrolled in this study.
-
Results
- SSI occurred in 15 of 44 patients (34.1%). The SSIs occurred more frequently in cases of repacking during the second-look surgery (0 vs. 4 [26.7%], P=0.010) and combined bladder-urethra injury (1 [3.4%] vs. 4 [26.7%], P=0.039). The incidence of SSIs was not significantly different between patients undergoing depacking within or after 48 hours (12 [41.4%] vs. 5 [33.3%], P=0.603). The mean time to diagnosis of SSI was 8.1±3.9 days from PPP. The most isolated organism was Staphylococcus epidermidis.
-
Conclusions
- Repacking and combined bladder-urethra injury are potential risk factors for SSI in patients with unstable pelvic fracture. Close observation is recommended for up to 8 days in patients with these risk factors. Further, 48 hours after PPP, removing the packed gauze on cessation of bleeding and not performing repacking can help prevent SSI. Additional analyses are necessary with a larger number of patients with the potential risk factors identified in this study.
-
Keywords: bone fractures; pelvic bone; surgical wound infection
INTRODUCTION
High-impact pelvic fracture is associated with greater than 30% morbidity and mortality due to associated retroperitoneal hemorrhage, postinjury coagulopathy, and traumatic-hemorrhagic shock despite various treatment modalities, including a multi-disciplinary team approach [1-3]. The concept of pelvic packing was first introduced by Pohlemann et al. [3] in 1994 in European trauma centers as a damage control resuscitation measure for patients with unstable pelvic fracture [4]. Recently, the Denver group modified the European modality of transabdominal pelvic packing as part of explorative laparotomy to a direct preperitoneal pelvic packing (PPP) technique through a separate suprapubic approach [5]. Recent studies demonstrated that PPP resulted in a significant decrease in need for transfusion and a lower rate of mortality [6-8]. However, infectious complications of PPP remain a major concern for physicians treating patients with trauma because the timing of definite surgery, such as open reduction, can be delayed, and the condition of critically ill patients can worsen owing to infectious complications after PPP.
Surgical site infection (SSI) is defined as a proliferation of pathogenic micro-organisms at the site of incision either within the skin and subcutaneous fat (superficial), musculofascial layers (deep), or in an organ or cavity opened during surgery [9]. SSI is one of the most common postoperative complications after laparotomy in abdominal trauma patients, with a reported incidence of 13.8% [10]. It can lead to wound dehiscence, hernia, and sepsis [11]. Many guidelines have suggested protocols to reduce the risk of SSI. Moreover, several studies were conducted to identify risk factors for SSI, and risk models were suggested to reduce SSI. However, as the suggested risk models were created for patients undergoing general and traumatic abdominal surgery [10,11], they were not applicable to patients undergoing PPP. Furthermore, few studies have been conducted to identify risk factors of SSI after PPP [3,4,6]; however, some of them primarily described risk factors for mortality and additionally reported risk factors for SSI [3,6].
We reported five patients with SSI after PPP in a 2018 study about the effectiveness of PPP in reducing mortality [3]. In this study, the risk factors for SSI occurring after PPP were investigated using patient data accumulated following the previous study.
MATERIALS AND METHODS
Patient Selection and Data Collection
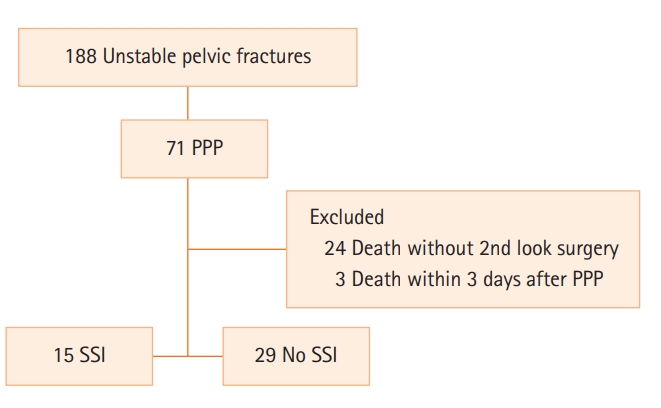
This retrospective study was approved by the Institutional Review Board of Wonju Severance Christian Hospital (IRB No. CR320202). The patient data were obtained from Wonju Severance Christian Hospital Pelvic Trauma Data Bank, in which data are prospectively maintained as part of the Korean Trauma Data Bank. Since the data were analyzed retrospectively and the identities of the patients were hidden, the requirement for informed consent was waived. The inclusion criteria were patients who (1) underwent PPP following unstable pelvic fracture, (2) were aged ≥18 years, and (3) agreed to collection and use of their medical information. Between April 2012 and May 2021, a total of 71 patients was enrolled. Hemodynamic instability was defined as persistent hypotension (systolic blood pressure [SBP] <90 mm Hg) despite administration of two units of packed red blood cells (pRBCs) [12,13]. The exclusion criteria were (1) death without second-look surgery and (2) death within 3 days after PPP. These patients were excluded because the survival time was too short to diagnose SSI. Based on the exclusion criteria, 44 patients were enrolled in this study (Figure 1). Data on patient characteristics of age, sex, initial SBP, cause of injury, history of diabetes mellitus, anticoagulant use, associated injury (abbreviated injury scale ≥2), concomitant bladder-urethra injury (BUI), concomitant bowel injury, injury severity score (ISS), laboratory data (initial hemoglobin level, lactate level, white blood cell count, and delta neutrophil index), pelvic fracture type (Young-Burgess and Tile classification), and presence of open fracture were collected. Data about patient management included use of a pelvic binder, use of resuscitative endovascular balloon occlusion of the aorta (REBOA), external fixator (EF) during PPP, screwing of the sacroiliac (SI) joint during PPP, open reduction and internal fixation (ORIF), whether PPP was performed in the emergency room (ER), time required to perform PPP, use of hemostatic gauze, time from accident to PPP, time from second-look surgery to drain removal, repacking during the second-look surgery, angioembolization after PPP, concomitant abdominal surgery, and pRBC transfusion during the first 4 hours after injury. Data about length of hospital stay, length of intensive care unit (ICU) stay, and mortality were collected. Details of SSI, including the source of sample for bacterial culture, time from first surgery to SSI was identified, and micro-organism detected on culture, were collected.
Patient Management
The Wonju Severance Christian Hospital has employed a trauma team since 2010, and the trauma center was constructed in January 2015. Until May 2014, pelvic binder application, massive transfusion, and pelvic angiography (PA) were performed in patients with a pelvic fracture with hemodynamic instability who showed contrast extravasation on computed tomography. After May 2014, PPP has been used in such cases. The orthopedic surgeons of the trauma team decided whether EF was necessary for the pelvic fracture and performed the procedure as appropriate. PA was performed if bleeding persisted after PPP and EF. REBOA has been performed in the ER in patients with trauma since February 2017, depending on the decision of the trauma team. A pelvic binder was applied by the trauma team in the ER to reduce pelvic volume and was removed just before PPP or PA. In cases requiring EF, the pelvic binders were not re-applied; conversely, they were reapplied just after PPP or the procedure in patients not requiring EF. Once the patients became hemodynamically stable, the pelvic binders were removed, and the trauma and orthopedic surgeons discussed the timing of definitive surgery for the pelvic fracture. After the initial transfusion with two units of O-negative pRBCs, cross-matched pRBCs, and fresh frozen plasma were administered in a 1 to 1 ratio according to our institution’s massive transfusion protocol.
PPP Technique
PPP was performed by trauma surgeons who had successfully completed the Definitive Surgical Trauma Care training provided by the International Association for Trauma Surgery and Intensive Care. After creating a 7–8 cm vertical skin incision beginning at the pubic symphysis, the anterior sheath of the rectus abdominis muscle was incised and the muscle was split. After the preperitoneal space was bluntly dissected in the posterolateral direction and the peritoneum moved to the medial side, the lower border of the SI joint was examined. Three surgical tapes were sequentially packed from the lower border of the SI joint using ringed forceps. This procedure was repeated on the contralateral side. After correction of coagulopathy, hypothermia, and metabolic acidosis, the packed surgical tapes were removed. One kaolin-impregnated gauze pad (QuikClot Combat Gauze; Z-medica, Wallingford, CT, USA) and two surgical tapes were used according to the decision of the trauma surgeon. After one QuikClot Combat Gauze was packed into the lower border of the SI joint, two surgical tapes were also packed. This procedure was repeated on the contralateral side. After packing, the anterior sheath of the rectus abdominis muscle and the skin were repaired.
Management after PPP
After correction of coagulopathy, metabolic acidosis, and hypothermia, the packed surgical gauze was removed according to the findings of the second-look surgery. The timing of tape removal was around 48 hours. After removal of the packed surgical gauze, a closed drain was routinely inserted into the site of the removed packed surgical gauze. The inserted drain was removed when the daily drain fluid amount was less than 60 ml. The timing of ORIF was determined in consultation with the orthopedic trauma staff.
Evaluation of SSI after PPP
Prophylactic antibiotics (second-generation cephalosporin) were administered preoperatively to patients who underwent PPP. The intravenous antibiotics were administered continuously until the second-look surgery in patients who underwent PPP. SSI was diagnosed according to the Centers for Disease Control and Prevention (CDC) guidelines [14]. Diagnostic criteria included purulent discharge from surgical site, microorganisms identified in tissue and fluid specimens, patient signs and symptoms, and abscess or other evidence of infection detected on imaging tests. SSI was evaluated by trauma surgeons after depacking. When SSI was clinically suspected, bacterial cultures of the open wound were performed. Discharge from wounds and drain fluid were also used for bacterial cultures to confirm SSI and isolate the bacterial species. Bacterial cultures were performed using drain fluid when SSI was clinically suspected based on drain fluid characteristics such as turbidity and foul odor with a clear wound.
Statistical Analysis
Continuous variables were compared using the Mann-Whitney U-test and are presented as mean±standard deviation or median (range). The chi-square test and Fisher’s exact test were used to compare categorical variables. A P-value <0.05 was considered statistically significant, and all statistical analyses were performed using IBM SPSS ver. 23.0 (IBM Corp., Armonk, NY, USA).
RESULTS
The mean age of the patients included in the study was 57.8±15.2 years; 27 patients (61.4 %) were male. The mean injury severity score was 37.5±8.0, and SSI occurred in 15 of 44 patients (34.1%).
Comparison between No SSI and SSI Groups
Concomitant BUI occurred significantly more often in the SSI group than in the no SSI group (4 [26.7%] vs. 1 [3.4%], P=0.039). There was no significant difference in the following variables between the no SSI and SSI groups: incidence of concomitant bowel injury (1 [ 3.4%] vs. 2 [13.3%], P=0.540), rate of open fracture (1 [3.4%] vs. 1 [6.7%], P=1.000), EF during PPP (4 [13.8%] vs. 4 [26.7%], P=0.414), time from PPP to tape removal (median, 45.0 vs. 41.3 hours; P=0.428), and time from second-look surgery to drain removal (median, 9 vs. 11 days; P=0.682). The proportion of patients in whom repacking was performed during second-look surgery was significantly higher in the SSI group than in the no SSI group (4 [26.7%] vs. 0, P=0.010). The rates of angioembolization after PPP (2 [6.9%] vs. 3 [20%], P=0.319) and combined abdominal surgery (5 [17.2%] vs. 3 [20.0%], P=1.000) were not different between the no SSI and SSI groups (Table 1).
Open Reduction and Internal Fixation
ORIF was performed with or a mean of 5.9±4.8 days after tape removal in 22 patients. ORIF was performed concomitant with tape removal in 4 of 22 patients. ORIF was not included in risk factor analysis for SSI because 18 cases underwent the procedure after tape removal.
Outcomes between No SSI and SSI Groups
Length of hospital stay (median, 41 vs. 64 days; P=0.480), length of ICU (median, 14 vs. 16 days; P=0.853), and mortality within 30 days (3 [10.3%] vs. 3 [20.0%], P=0.394) were not significantly different between the groups (Table 2).
Timing of Tape and Drain Removal and SSI
There was no difference in the rate of SSI between those who underwent depacking within or after 48 hours after PPP (12 [41.4%] vs. 5 [33.3%], P=0.603). There was no difference in rate of SSI between those who underwent drain removal within or after 7 days after depacking (18 [62.1%] vs. 8 [53.3%], P=0.576) (Table 3).
Details of Patients with SSI
Bacteria were isolated from wounds in 10 patients and from drain fluid in 6 patients. Bacteria were identified simultaneously in both wound and drain fluid in one patient. The mean period to detection of SSI from PPP was 8.1±3.9 days. The most common bacteria cultured was Staphylococcus epidermidis (Table 4).
DISCUSSION
This study showed that repacking during second-look surgery and concomitant BUI were potential risk factors for SSI. Burlew et al. [6] reported different rates of infection in the pelvic space between those requiring repacking (9 of 20 patients, 45%) and those who underwent single packing (6 of 108 patients, 6%) [6]. Based on the results of Burlew et al. [6], the Denver group modified their PPP protocol to avoid repacking despite continuing hemorrhage, with a focus on early reversal of post-injury coagulopathy and secondary angioembolization in cases of ongoing blood product requirements or known source of arterial bleeding [4]. All repacking in our institution was performed during second-look surgery. Because gauze repacked in the same space can promote bacterial colonization, clean gauze was used for repacking. Therefore, we also recommend that repacking be avoided by controlling the ongoing hemorrhage after PPP with the aid of angiography and appropriate correction of coagulopathy in the ICU.
The study by the Denver group also demonstrated associated bladder injury as a specific risk factor for pelvic space infection [6]. The CDC guidelines [15] only mention that usage of prophylactic antibiotics in urological operations “may not be beneficial if urine is sterile.” This suggests that sterile urine might not be associated with SSI. A study that investigated SSI in elective urologic surgery showed that the occurrence of SSI in urologic surgery was associated with preoperative urinary tract infection (UTI) because one of the characteristics of urologic operations is leakage of non-sterile urine into the surgical field, causing contamination [16]. However, nine patients in that study who developed SSI did not experience preoperative UTI [16]. The exact mechanism of development of SSI with sterile urine has not yet been identified. Since it was not possible to confirm whether patients enrolled in this study had UTI before the ER visit, we could not explain how urinary leakage affected SSI. However, since BUI with pelvic injury indicates more severe injuries compared to pelvic injury without BUI, and severe trauma is associated with altered host defense, characterized by early hyperinflammation, followed by immunosuppression and enhanced susceptibility to infection [17-19], patients with pelvic injury and BUI might be more susceptible to infection.
Our study showed that open fracture was not associated with SSI. Previous studies demonstrated that open pelvic fractures have an increased risk of SSIs compared to closed pelvic ring injuries [20-22]. The results of this study were different from those of previous studies possibly because of the smaller number of patients recruited over a shorter period.
SSI occurred in two patients with concomitant bowel injury and pelvic fracture. If simultaneous PPP and laparotomy are necessary, a separate laparotomy incision should be created from that for packing to avoid wound contamination and optimally should be located above the umbilicus to prevent penetration of the preperitoneal space. However, the same low midline incision was used for PPP and laparotomy in the two patients because they had a perforation of the rectum and descending colon. Although bowel injury was not a risk factor for SSI in this study, bowel injury is an important factor to reduce SSI. Therefore, a transverse incision (Pfannenstiel) for PPP might be useful for patients who need to undergo laparotomy through a low midline incision simultaneously with PPP [23].
Once acute hemorrhage is under control in patients with hemodynamic instability due to pelvic fracture, trauma surgeons must make the important decision about when to remove the packing tape. In addition, trauma surgeons need to decide the optimal timing of drain removal to prevent SSI. The timing of packed gauze removal was recommended as 24–48 hours after PPP in most previous studies; however, it was not based on evidence but experience [13,24]. There was no difference in the rate of SSI between those who underwent depacking within or after 48 hours after PPP. Stahel et al. [4] reported that the two patients who had SSI underwent pelvic depacking after longer than 48 hours. However, one of them underwent angioembolization after pelvic packing, resulting in perineal and anorectal necrosis. This result does not show a definite correlation between SSI and time from PPP to tape removal. Trauma surgeons tend to remove the drain within 7 days after tape removal to avoid introduction of a foreign body reaction, which might aggravate the infection and stimulate collagenolysis [25], and the risk of ascending infection might increase. However, the duration from second-look surgery to drain removal was not associated with SSI, and there was no difference in rate of SSI between those in whom the drain was removed before or after 7 days. More evidence about optimal timing of tape and drain removal is necessary in the future.
Our previous study showed an SSI rate of 20% (5 of 25 patients who underwent PPP) [3]. Burlew et al. [6] reported that the rate of infection of the pelvic space after PPP was 12%. Li et al. [26] reported a rate of SSI of 10% (3 of 29 patients who underwent PPP). Another study demonstrated a rate of infection as high as 28% [8], while our study showed a rate of SSI of 34.1%. One of the difficulties in analysis of pelvic trauma management is reflected in the characteristics of the patient population [6]. The mean age of patients enrolled in this study was 57.8±15.2 years, which was higher than that of the populations in other studies. A study conducted to identify risk factors for SSI in patients with abdominal trauma reported age as one of the factors contributing to SSI [11]. Therefore, the higher rate of infection might be relatively acceptable considering the mean patient age in our study.
In our data, the mean duration to SSI from PPP was 8.1 days. Our previous study reported a mean duration of 7.8 days. Li et al. [26] identified deep SSI after 7–9 days. These results are similar to those of the current study and suggest that trauma physicians should be alert to the occurrence of SSI after especially 7–9 days of admission. Our data demonstrated that SSI was not associated with angioembolization. Only one patient who underwent nonselective angioembolization of the internal iliac artery after PPP in our study was diagnosed with SSI. Selective or super-selective embolization was performed in a branch of the internal iliac artery for the remaining four patients. One study demonstrated nonselective angioembolization as one of the risk factors for SSI [27]. Burlew et al. [6] suggested that empiric embolization of both internal iliac arteries should be carefully weighed against the risks of pelvic claudication and perineal necrosis. Obviously, angioembolization is an effective, timesaving, and readily available procedure for pelvic fracture-related arterial hemorrhage. However, given the high rate of SSI, trauma physicians should be careful in deciding on nonselective angioembolization.
This study has some limitations. First, the number of enrolled patients was small, and the study design was retrospective. Second, this study was performed at a single trauma center, and the demographics of our patient population and surgical treatment concepts cannot be generalized and extrapolated to the entire population.
In conclusion, repacking and combined BUI are potential risk factors for SSI in patients with unstable pelvic fracture after PPP. Additional analyses are necessary with a larger number of patients using the potential risk factors identified in this study. Based on our study, SSI usually occurs around 8 days after PPP. Therefore, close observation is recommended in patients with these risk factors for about 8 days after injury. In particular, avoiding repacking and controlling hemorrhage using angiography and adequate correction of coagulopathy in the ICU can reduce the risk of SSI. Although it commonly is suggested that packing tape be removed as soon as possible, the results of this study suggest that there is no need to stress over removal of packing tape within 48 hours. Rather, removing the packing tape after bleeding has stopped and not performing repacking might help prevent SSI.
HIGHLIGHTS
▪ Repacking and combined bladder-urethra injury are potential risk factors for surgical-site infection in patients with unstable pelvic fracture.
▪ Close observation is recommended for up to 8 days in patients with these risk factors.
▪ At 48 hours after preperitoneal pelvic packing, removing the packed gauze on cessation of bleeding and not performing repacking can help prevent surgical site infection.
NOTES
-
CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
Conceptualization: KMK, JYJ, KK. Data curation: JSC, JWK, MJK, YUC, HS, KK. Formal analysis: KMK, KK. Methodology: KMK, KK. Project administration: JSC, JWK, MJK, YUC, HS, JYJ, KSB, KK. Visualization: KMK, MJK, KK. Writing–original draft: KMK, MJK, KK. Writing–review & editing: all authors.
Acknowledgments
We would like to thank all trauma surgeons and nurses for their dedication and commitment to the Korean trauma system.
Figure 1.Patient flowchart. PPP: preperitoneal pelvic packing; SSI: surgical-site infection.

Table 1.Comparison between no SSI and SSI groups
|
Variable |
No SSI (n=29) |
SSI (n=15) |
P-value |
|
Age (yr) |
59.2±13.5 |
55.2±18.3 |
0.655 |
|
Male |
17 (58.6) |
10 (66.7) |
0.603 |
|
Initial SBP (mm Hg) |
68.7±11.8 |
58.6±21.0 |
0.161 |
|
Cause of injury |
|
|
0.216 |
|
Traffic collision |
9 (31.0) |
2 (13.3) |
|
|
Pedestrian struck |
9 (31.0) |
8 (53.3) |
|
|
Fall |
10 (34.5) |
3 (20.0) |
|
|
Other blunt trauma |
1 (3.4) |
1 (6.7) |
|
|
Unknown |
0 |
1 (6.7) |
|
|
DM |
5 (17.2) |
3 (20.0) |
1.000 |
|
Use of anticoagulants |
2 (6.9) |
2 (13.3) |
0.596 |
|
Associated injury (AIS ≥2) |
26 (89.7) |
14 (93.3) |
1.000 |
|
Concomitant bladder-urethra injury |
1 (3.4) |
4 (26.7) |
0.039 |
|
Concomitant bowel injury |
1 (3.4) |
2 (13.3) |
0.540 |
|
Injury severity score |
37.7±8.8 |
37.1±6.6 |
0.891 |
|
Initial Hb (g/dl) |
9.3±2.0 |
10.5±2.0 |
0.063 |
|
Initial lactate (mmol/L) |
5.2±2.8 |
7.6±4.3 |
0.055 |
|
Initial WBC (×109/L) |
14,207±4,874 |
13,414±5,304 |
0.561 |
|
Initial DNI (%) |
2.0±2.6 |
1.6±2.4 |
0.735 |
|
YB classification |
|
|
0.229 |
|
LC |
19 (65.5) |
7 (46.7) |
|
|
APC |
2 (6.9) |
4 (26.7) |
|
|
VS |
8 (27.6) |
4 (26.7) |
|
|
Tile classification |
|
|
0.431 |
|
A |
0 |
0 |
|
|
B |
19 (65.5) |
8 (53.3) |
|
|
C |
10 (34.5) |
7 (46.7) |
|
|
Open fracture |
1 (3.4) |
1 (6.7) |
1.000 |
|
Pelvic binder |
12 (41.4) |
10 (66.7) |
0.112 |
|
REBOA |
0 |
2 (13.3) |
0.111 |
|
EF during PPP |
4 (13.8) |
4 (26.7) |
0.414 |
|
SI joint screwing during PPP |
4 (13.8) |
2 (13.3) |
1.000 |
|
PPP in ER |
1 (3.4) |
3 (20.0) |
0.107 |
|
Median time required to perform PPP (min) |
35 |
25 |
0.333 |
|
Use of hemostatic gauze |
12 (41.4) |
5 (33.3) |
0.603 |
|
Median time from accident to PPP (min) |
275 |
190 |
0.122 |
|
Median time from PPP to tape removal (hr) |
45 |
41.3 |
0.428 |
|
Median time from 2nd look surgery to drain removal (day) |
9 |
11 |
0.682 |
|
Repacking during 2nd look surgery |
0 |
4 (26.7) |
0.010 |
|
Angioembolization after PPP |
2 (6.9) |
3 (20.0) |
0.319 |
|
Combined abdominal surgery |
5 (17.2) |
3 (20.0) |
1.000 |
|
pRBC transfusion during first 4 hours |
8.5±4.7 |
8.5±8.0 |
0.417 |
Table 2.Comparison of outcomes between no SSI and SSI groups
|
Variable |
No SSI (n=29) |
SSI (n=15) |
P-value |
|
Median length of hospital stay (day) |
41 |
64 |
0.480 |
|
Median length of ICU stay (day) |
14 |
16 |
0.853 |
|
Mortality within 30 days, n (%) |
3 (10.3) |
3 (20.0) |
0.394 |
Table 3.Comparative analysis between the no SSI and SSI groups for timing of removal of tape and drain
|
Variable |
Time |
No SSI (n=29) |
SSI (n=15) |
P-value |
|
Time from PPP to tape removal (hr) |
≥48 |
12 (41.4) |
5 (33.3) |
0.603 |
|
Time from 2nd look surgery to drain removal (day) |
≥7 |
18 (62.1) |
8 (53.3) |
0.576 |
Table 4.Details of patients with SSI
|
No |
Source of culture |
Time of detection of SSI from the time of PPP (day) |
Organism isolated |
|
1 |
Wound |
13 |
Staphylococcus epidermidis, Acinetobacter baumannii
|
|
2 |
Wound |
12 |
Staphylococcus aureus, Enterobacter aerogenes
|
|
3 |
Drain fluid |
6 |
Enterococcus faecalis
|
|
4 |
Wound |
8 |
Enterococcus casseliflavus
|
|
5 |
Drain fluid |
3 |
Enterococcus faecium
|
|
Klebsiella pneumoniae
|
|
6 |
Wound |
6 |
Escherichia coli
|
|
7 |
Wound |
3 |
S. epidermidis
|
|
8 |
Drain fluid |
3 |
S. epidermidis
|
|
9 |
Wound |
9 |
Methicillin-resistant Staphylococcus aureus
|
|
Micrococcus kristinae
|
|
A. baumannii
|
|
10 |
Wound |
12 |
S. epidermidis
|
|
E. faecium
|
|
11 |
Drain fluid, Wound |
9 |
Corynebacterium striatum
|
|
12 |
Drain fluid |
13 |
A. baumannii
|
|
13 |
Wound |
6 |
Pus discharged |
|
No result of culture |
|
14 |
Drain fluid |
14 |
C. striatum
|
|
15 |
Wound |
5 |
S. epidermidis
|
|
Staphylococcus lugdunensis
|
References
- 1. Costantini TW, Coimbra R, Holcomb JB, Podbielski JM, Catalano R, Blackburn A, et al. Current management of hemorrhage from severe pelvic fractures: results of an American Association for the Surgery of Trauma multi-institutional trial. J Trauma Acute Care Surg 2016;80:717-23.PubMed
- 2. Kim TH, Yoon YC, Chung JY, Song HK. Strategies for the management of hemodynamically unstable pelvic fractures: from preperitoneal pelvic packing to definitive internal fixation. Asian J Surg 2019;42:941-6.ArticlePubMed
- 3. Pohlemann T, Gänsslen A, Bosch U, Tscherne H. The technique of packing for control of hemorrhage in complex pelvis fractures. Tech Orthop 1995;9:267-70.ArticlePubMedPMC
- 4. Stahel PF, Moore EE, Burlew CC, Henderson C, Peña AJ, Harry D, et al. Preperitoneal pelvic packing is not associated with an increased risk of surgical site infections after internal anterior pelvic ring fixation. J Orthop Trauma 2019;33:601-7.ArticlePubMed
- 5. Smith WR, Moore EE, Osborn P, Agudelo JF, Morgan SJ, Parekh AA, et al. Retroperitoneal packing as a resuscitation technique for hemodynamically unstable patients with pelvic fractures: report of two representative cases and a description of technique. J Trauma 2005;59:1510-4.ArticlePubMed
- 6. Burlew CC, Moore EE, Stahel PF, Geddes AE, Wagenaar AE, Pieracci FM, et al. Preperitoneal pelvic packing reduces mortality in patients with life-threatening hemorrhage due to unstable pelvic fractures. J Trauma Acute Care Surg 2017;82:233-42.ArticlePubMedPMC
- 7. Moskowitz EE, Burlew CC, Moore EE, Pieracci FM, Fox CJ, Campion EM, et al. Preperitoneal pelvic packing is effective for hemorrhage control in open pelvic fractures. Am J Surg 2018;215:675-7.ArticlePubMed
- 8. Petrone P, Rodríguez-Perdomo M, Pérez-Jiménez A, Ali F, Brathwaite C, Joseph DK. Pre-peritoneal pelvic packing for the management of life-threatening pelvic fractures. Eur J Trauma Emerg Surg 2019;45:417-21.ArticlePubMed
- 9. Dessie W, Mulugeta G, Fentaw S, Mihret A, Hassen M, Abebe E. Pattern of bacterial pathogens and their susceptibility isolated from surgical site infections at selected referral hospitals, Addis Ababa, Ethiopia. Int J Microbiol 2016;2016:2418902. ArticlePubMedPMC
- 10. Morales CH, Escobar RM, Villegas MI, Castaño A, Trujillo J. Surgical site infection in abdominal trauma patients: risk prediction and performance of the NNIS and SENIC indexes. Can J Surg 2011;54:17-24.ArticlePubMedPMC
- 11. Isbell KD, Hatton GE, Wei S, Green C, Truong V, Woloski J, et al. Risk stratification for superficial surgical site infection after emergency trauma laparotomy. Surg Infect (Larchmt) 2021;22:697-704.ArticlePubMedPMC
- 12. Perkins ZB, Maytham GD, Koers L, Bates P, Brohi K, Tai NR. Impact on outcome of a targeted performance improvement programme in haemodynamically unstable patients with a pelvic fracture. Bone Joint J 2014;96:1090-7.ArticlePubMed
- 13. Coccolini F, Stahel PF, Montori G, Biffl W, Horer TM, Catena F, et al. Pelvic trauma: WSES classification and guidelines. World J Emerg Surg 2017;12:5. ArticlePubMedPMC
- 14. National Healthcare Safety Network. Surgical site infection event (SSI) [Internet]. Atlanta (GA): Centers for Disease Control and Prevention; 2021 [Epub]. Available from: http://www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf.
- 15. Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR. Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol 1999;20:250-78.PubMed
- 16. Hamasuna R, Betsunoh H, Sueyoshi T, Yakushiji K, Tsukino H, Nagano M, et al. Bacteria of preoperative urinary tract infections contaminate the surgical fields and develop surgical site infections in urological operations. Int J Urol 2004;11:941-7.ArticlePubMed
- 17. Keel M, Trentz O. Pathophysiology of polytrauma. Injury 2005;36:691-709.ArticlePubMed
- 18. Hietbrink F, Koenderman L, Rijkers G, Leenen L. Trauma: the role of the innate immune system. World J Emerg Surg 2006;1:15. ArticlePubMedPMC
- 19. Stahel PF, Smith WR, Moore EE. Role of biological modifiers regulating the immune response after trauma. Injury 2007;38:1409-22.ArticlePubMed
- 20. Hermans E, Edwards M, Goslings JC, Biert J. Open pelvic fracture: the killing fracture? J Orthop Surg Res 2018;13:83. ArticlePubMedPMC
- 21. Siada SS, Davis JW, Kaups KL, Dirks RC, Grannis KA. Current outcomes of blunt open pelvic fractures: how modern advances in trauma care may decrease mortality. Trauma Surg Acute Care Open 2017;2:e000136. ArticlePubMedPMC
- 22. Song W, Zhou D, Xu W, Zhang G, Wang C, Qiu D, et al. Factors of pelvic infection and death in patients with open pelvic fractures and rectal injuries. Surg Infect (Larchmt) 2017;18:711-5.ArticlePubMed
- 23. Kim DH, Chang YR. Preperitoneal pelvic packing. Trauma Image Proc 2017;42-3.Article
- 24. Burlew CC, Moore EE, Smith WR, Johnson JL, Biffl WL, Barnett CC, et al. Preperitoneal pelvic packing/external fixation with secondary angioembolization: optimal care for life-threatening hemorrhage from unstable pelvic fractures. J Am Coll Surg 2011;212:628-35.ArticlePubMed
- 25. Leaper DJ. Risk factors for surgical infection. J Hosp Infect 1995;30 Suppl:127-39.ArticlePubMed
- 26. Li Q, Dong J, Yang Y, Wang G, Wang Y, Liu P, et al. Retroperitoneal packing or angioembolization for haemorrhage control of pelvic fractures: quasi-randomized clinical trial of 56 haemodynamically unstable patients with Injury Severity Score ≥33. Injury 2016;47:395-401.ArticlePubMed
- 27. Lai CY, Tseng IC, Su CY, Hsu YH, Chou YC, Chen HW, et al. High incidence of surgical site infection may be related to suboptimal case selection for non-selective arterial embolization during resuscitation of patients with pelvic fractures: a retrospective study. BMC Musculoskelet Disord 2020;21:335. ArticlePubMedPMC
Citations
Citations to this article as recorded by

- Angioembolization Has Similar Efficacy and Lower Total Charges than Preperitoneal Pelvic Packing in Patients With Pelvic Ring or Acetabulum Fractures
Aaron Singh, Travis Kotzur, Ezekial Koslosky, Rishi Gonuguntla, Lorenzo Canseco, David Momtaz, Ali Seifi, Case Martin
Journal of Orthopaedic Trauma.2024; 38(5): 254. CrossRef - Factors Associated With Pelvic Infection After Pre-Peritoneal Pelvic Packing for Hemodynamically Unstable Pelvic Fractures
Jennifer E. Baker, Husayn A. Ladhani, Caitlyn McCall, Chelsea R. Horwood, Nicole L. Werner, Barry Platnick, Clay Cothren Burlew
Surgical Infections.2024; 25(5): 399. CrossRef - Comparison of Conventional versus Modified Preperitoneal Pelvic Packing in Patients with Bleeding Pelvic Fractures: A Single-Center Retrospective Pilot Study
Sebeom Jeon, Byungchul Yu, Gil Jae Lee, Min A Lee, Jungnam Lee, Kang Kook Choi
Journal of Clinical Medicine.2024; 13(14): 4062. CrossRef - Current Management of Hemodynamically Unstable Patients with Pelvic Fracture
Kevin Harrell, Chelsea Horwood, Clay Cothren Burlew
Current Surgery Reports.2023; 11(4): 92. CrossRef - Open Fixation After Preperitoneal Pelvic Packing Is Associated With a High Surgical Site Infection Rate
Ye Joon Kim, Bryan L. Scott, Fredric M. Pieracci, Ernest E. Moore, Cyril Mauffrey, Joshua A. Parry
Journal of Orthopaedic Trauma.2023; 37(11): 547. CrossRef - Extraperitoneal pelvic packing in trauma – a review
Sajad Ahmad Salati
Polish Journal of Surgery.2022; 95(3): 46. CrossRef
 , Myoung Jun Kim2,3,4
, Myoung Jun Kim2,3,4 , Jae Sik Chung2,3,4
, Jae Sik Chung2,3,4 , Ji Wool Ko2,3,4
, Ji Wool Ko2,3,4 , Young Un Choi2,3,4
, Young Un Choi2,3,4 , Hongjin Shim2,3,4
, Hongjin Shim2,3,4 , Ji Young Jang5
, Ji Young Jang5 , Keum Seok Bae2,3
, Keum Seok Bae2,3 , Kwangmin Kim2,3,4
, Kwangmin Kim2,3,4







 KSCCM
KSCCM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite