Abstract
-
Background
- Medical emergency teams (METs) have shown their merit in preventing unexpected cardiac arrest. However, it might be impractical for small- or medium-sized hospitals to operate an MET due to limited manpower and resources. In this study, we sought to evaluate the feasibility of a medical alert system (MAS) that alerts all doctors involved in patient care of patient deterioration via text message using smart-phones.
-
Methods
- The MAS was test-operated from July 2015 to September 2015, in five general wards with a high incidence of cardiac arrest. The number of cardiac arrests was compared to that of 2014. The indication for activation of MAS was decided by the intensive care unit committee of the institution, which examined previous reports on MET.
-
Results
- During the three-month study period, 2,322 patients were admitted to the participating wards. In all, MAS activation occurred in 9 patients (0.39%). After activation, 7 patients were admitted to the intensive care unit. Two patients (0.09%) experienced cardiac arrest. Of 13,129 patients admitted to the ward in 2014, there were 50 cases (0.38%) of cardiac arrest (p = 0.009).
-
Conclusions
- It is feasible to use MAS to prevent unexpected cardiac arrest in a general ward.
-
Keywords: heart arrest; hospital rapid response team; mortality
Introduction
Although medical technology has advanced greatly, cardiac arrest (CA) of patients admitted to hospitals still occurs in subpopulation of patients admitted to hospitals. CA not only worsens patient’s outcome, but also might aggravate anxiety of nearby patients and their families weakening rapport with and confidence on the medical team.
To prevent CA, many hospitals have started to operate medical emergency team (MET). The rationale behind MET is that many patients experiencing CA show abnormal vital signs or neurologic changes such as, altered mental status at six to eight hours before these critical events [1,2]. The goal of MET is to try to catch these changes and respond to patients rapidly to prevent CA. The MET have been shown to improve patient outcome in several studies [3-5]. It has also shown feasibility in Korea [6,7].
However, it is difficult for a small rural hospital to run MET due to limited manpower and financial burden to run a specialized team. Therefore, we prepared a medical alerting system (MAS) for a small rural hospital. Instead of calling a specialized MET to rescue deteriorating patients, MAS was set up to send out alerting messages to every doctor participating in patient care (from intern to staff) concurrently via smart phone when the patient meet activation criteria of MAS. To verify the effect of MAS in reducing unexpected CA following cardiopulmonary resuscitation (CPR) in a general ward (GW), we performed this pilot study before its overall implementation.
Materials and Methods
The present study was performed at a 700-bed secondary hospital which has about 1,400 employees. It is located at a rural city of 430,000 residents. It is a training hospital for internship and residentship. There were about 2.87 patients per each nurse on general ward averagely. Institutional Review Board approved this study. Informed consent was waived.
Five GW’s with highest occurrence rates of CPR were selected by analyzing rates of CA of individual wards in 2014. The patients in the five wards were generally under care of cardiology, oncology, pulmonology, nephrology, neurology, and trauma surgery departments. There were a total of 240 beds in the wards. MAS was test-operated about from July 2015 to September 2015.
This study included adult patients who were admitted to these 5 GW. Pediatric patients younger than 15 years old were excluded. And patients with certain possibility of mortality were excluded because this study focused on the reduction of unexpected CPR in a GW. Therefore CA at intensive care unit (ICU) or emergency room were excluded because patients in those place were in critical condition and had some potential of CA. In addition, hopeless patients and patients with do-not-rescue situation were excluded. The indication for activation of MAS was decided by intensive care unit committee of the institution which examined previous reports on MET [6,7]. Lung, heart, and nervous system related abnormal symptoms and signs were included in the indications. The medical team was allowed to activate MAS even if the patient did not meet the activation criteria if they were concerned about patient’s well-being (Table 1).
The nurse in charge of patient care was instructed to activate MAS when the patient in charge met the activation criteria for MAS. The MAS was incorporated into the hospital electronic record system and when activated sent patient’s name, room number, and abnormal findings via smart phone message to all the doctors involved in patient care concurrently. There was no pre-specified protocol about what the doctors had to do once the MAS was activated and treatment decisions were left to clinical teams.
MAS was introduced to hospital staff via e-mails and posters. The quality improvement team of the hospital educated unit managers of the wards, residents, and interns.
The proportion of CPR, MAS activation and admissions were checked. The number of CPR and admitted patients in 2014 were used as control group.
Chi-squared and Fisher’s exact tests were used for qualitative comparison. A p-value of less than 0.05 was considered as statistically significant.
Results
During the test-operating period in 2015, 2,322 patients were admitted to selected wards. There were 9 cases (0.39%) of MAS activation and among them seven patients were transferred to the intensive care unit. Two patients experienced CA despite MAS activation. Overall mortality for these patients was 33.3% (3/9) Detailed information of these activations are summarized in Table 2.
From January to December of 2014, 13,129 patients were admitted to five selected wards (Table 3). There were 199 cases of mortality and 50 cases (0.38%) of cardiopulmonary resuscitation at the wards. MAS was activated similarly for control period. However, cardiac arrest showed significant reduction (p = 0.009; odds ratio: 0.226; 95% confidence interval: 0.055 to 0.931)
Discussion
In this study, we confirm the feasibility of MAS in decreasing the incidence of CA in GW’s in a medium sized training hospital in Korea. In Korea, intern and junior residents with little clinical experience and medical knowledge are usually charged with care of in-patients. When a patient deteriorates, these doctors and nurses might misjudge the importance of patient’s change leading to CA. MET is a specialized team in the hospital to help the medical teams in managing critically-ill patients so that they do not experience adverse outcome [8,9]. But to operate a MET, you need doctors with sufficient clinical experience and medical knowledge along with other resources, which a medium-sized hospital do not have.
We designed the MAS based on critical value reporting (CVR) system in the electronic medical record system. CVR system is a system that reports potentially critical laboratory results to responsible physicians urgently to improve patient’s outcome [10]. It has been reported that this system could make changes of treatment plan in two-third of patients [11]. We thought that just reporting potentially critical sign or symptom of patients might be able to change treatment plan and improve patient’s outcome. In addition, we hypothesized that if absolute indications for activation of MAS are specified, it would be hard to ignore them (Table 1).
After implementation of work hour restriction on trainees, smaller numbers of doctors are on call at night. Doctors on duty at night might not be able to properly evaluate each patient’s condition and problems. Therefore, they might not be able to respond properly. In addition, on-call junior doctors in the classic system might be performing procedure or operation so that they could not respond to ward’s notification immediately. Concurrent reporting of MAS which gives messages to all doctors involved in patient care might enable proper management for such situation without requiring additional step (Figure 1), thus enabling and promoting higher level of care [12].
MAS has a limitation in some situations. In some hospitals with tendency to suppress consultation to other department or hesitate do-not-resuscitate order in hopeless terminal patients, MAS might be ineffective. Also even if they are notified of patient’s deterioration, doctors might not be able to manage patients properly. Unlike specialized MET staffs, almost all doctors in MAS are not specialized for critical care. However, they could consult pertinent departments and ask for help urgently so that patients’ outcome could be improved.
The present study has some limitations. It analyzed only CA in GW, while other studies analyzed other important outcomes as mortality, unexpected ICU admission, and so on. The present study is a small feasibility study and other outcomes should be investigated in the future. In addition, there are possibilities of bias and confounding when selecting the intervention and control groups. Especially since during the intervention period Korea experienced Middle East Resiratory Syndrome with change in patient mix which we were not able to measure.
In conclusion, it might be feasible to use MAS to prevent unexpected CA in a GW. However, this pilot study was performed for a short period. Based on the result of this study, MAS has been applied to all the wards in our hospital. Further analysis of its long-term result with other factors such as mortality and unexpected ICU admission is needed to evaluate the effectiveness of MAS in improving patient outcome.
NOTES
-
No potential conflict of interest relevant to this article was reported.
Figure 1.Algorithm of the medical alert system. Under specific conditions, it rules automatic reporting concurrently. Therefore, the system prevents important changes from being ignored and reduces the time to properly manage cardiac events.
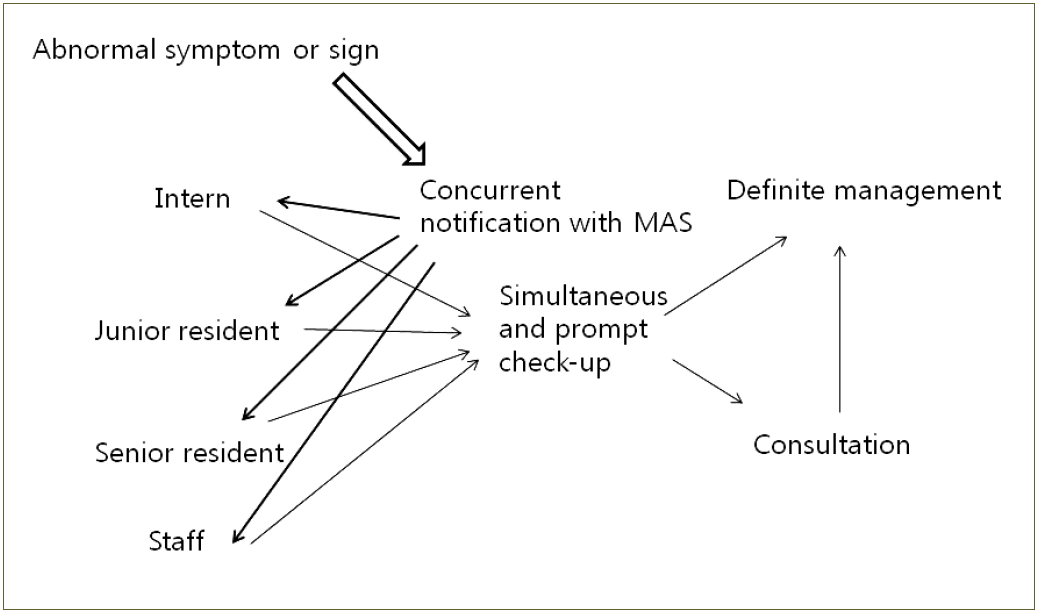
Table 1.Indications for activation of MAS (MAS will be activated with any one condition)
|
Criteria |
Parameters |
|
Respiratory |
Respiratory rate ≤ 8/minute, ≥ 24/minute |
|
Ongoing hypoxia (SaO2 ≤ 90%) more than 5 minutes |
|
pH < 7.2 |
|
PaO2 < 55 mmHg |
|
PaCO2 > 55mmHg |
|
Cardiology |
Symptomatic hypotension (systolic blood pressure ≤ 85 mmHg) |
|
Pulse rate ≤ 50/minute, ≥ 120/minute |
|
Neurologic |
Sudden change of mental status |
|
Sudden agitation |
|
Seizure |
|
Other |
Any other anxious condition |
Table 2.Comparison of cardiac arrest in the MAS test-operating period and the control period
|
Patient No. |
Sex |
Age |
Diagnosis |
Reason of MAS activation |
Management |
ICU Adm |
CPR |
Mortality |
|
1 |
M |
83 |
Heart failure |
Hypoxia |
Oral suction, Oxygenation |
Y |
N |
Y |
|
2 |
F |
75 |
Pneumonia |
Other anxious condition |
Oral suction, Oxygenation |
N |
N |
N |
|
3 |
M |
73 |
Pneumonia |
Tachycardia |
Oral suction, Oxygenation |
Y |
N |
N |
|
4 |
M |
76 |
Myocardial infarction |
Bradycardia |
Intubation, CPR |
Y |
Y |
Y |
|
5 |
F |
78 |
Pneumonia |
Hypoxia |
Oral suction, Oxygenation |
N |
N |
N |
|
6 |
M |
53 |
Fiver cirrhosis |
Hypoxia |
Intubation, CPR |
Y |
Y |
Y |
|
7 |
M |
30 |
Acute pancreatitis |
Hypoxia, Tachycardia |
Centrallineinsertion, Massive hydration |
Y |
N |
N |
|
8 |
N/A |
N/A |
N/A |
Decreased Mentality |
N/A |
Y |
N |
N |
|
9 |
N/A |
N/A |
Acute kidney injury |
Other anxious condition |
Continuous renal replacement |
Y |
N |
N |
Table 3.Comparison of cardiac arrest in MAS test-operating period and the control period
|
Case |
Control period |
MAS test-operating period |
p-value |
OR (95% CI) |
|
Admission |
13,179 |
2,322 |
|
|
|
Mortality |
199 (1,49) |
27 (1,15) |
0,204 |
|
|
MAS activation |
|
9 (0,39) |
> 0,99 |
|
|
CPR |
50 (0,38) |
2 (0,09) |
0,009 |
0,226 (0,050-0,931) |
References
- 1. Schein RM, Hazday N, Pena M, Ruben BH, Sprung CL. Clinical antecedents to in-hospital cardiopulmonary arrest. Chest 1990;98:1388-92.ArticlePubMed
- 2. Smith AF, Wood J. Can some in-hospital cardio-respiratory arrests be prevented? A prospective survey. Resuscitation 1998;37:133-7.ArticlePubMed
- 3. Buist MD, Moore GE, Bernard SA, Waxman BP, Anderson JN, Nguyen TV. Effects of a medical emergency team on reduction of incidence of and mortality from unexpected cardiac arrests in hospital: preliminary study. BMJ 2002;324:387-90.ArticlePubMedPMC
- 4. Bellomo R, Goldsmith D, Uchino S, Buckmaster J, Hart GK, Opdam H, et al. A prospective before-and-after trial of a medical emergency team. Med J Aust 2003;179:283-7.ArticlePubMed
- 5. Bellomo R, Goldsmith D, Uchino S, Buckmaster J, Hart G, Opdam H, et al. Prospective controlled trial of effect of medical emergency team on postoperative morbidity and mortality rates. Crit Care Med 2004;32:916-21.ArticlePubMed
- 6. Kwak HJ, Yun I, Kim SH, Sohn JW, Shin DH, Yoon HJ, et al. The extended rapid response system: 1-year experience in a university hospital. J Korean Med Sci 2014;29:423-30.ArticlePubMedPMC
- 7. Joo H, Park SH, Hong SB, Lim CM, Koh Y, Lee YS, et al. Usefulness of screening criteria system used by medical alert team in a general hospital. Korean J Crit Care Med 2012;27:151-6.Article
- 8. Alam N, Hobbelink EL, van Tienhoven AJ, van de Ven PM, Jansma EP, Nanayakkara PW. The impact of the use of the Early Warning Score (EWS) on patient outcomes: a systematic review. Resuscitation 2014;85:587-94.ArticlePubMed
- 9. Tobin AE, Santamaria JD. Medical emergency teams are associated with reduced mortality across a major metropolitan health network after two years service: a retrospective study using government administrative data. Crit Care 2012;16:R210. ArticlePubMedPMC
- 10. Dighe AS, Rao A, Coakley AB, Lewandrowski KB. Analysis of laboratory critical value reporting at a large academic medical center. Am J Clin Pathol 2006;125:758-64.ArticlePubMed
- 11. Howanitz PJ, Steindel SJ, Heard NV. Laboratory critical values policies and procedures: a college of American Pathologists Q-Probes Study in 623 institutions. Arch Pathol Lab Med 2002;126:663-9.ArticlePubMed
- 12. Findlay GP, Shotton H, Kelly K, Mason M. Time to Intervene? A review of patients who underwent cardopulmonary resuscitation as a result of an inhospital cardiorespiratory arrest. London, National Confidentail Enquiry into Patient Outcome and Death. 2012, pp 1-125.
Citations
Citations to this article as recorded by








 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite


