Abstract
-
Background:
- The aim of this study was to investigate the effects of using a systematic approach to tracheostomy care by a clinical nurse specialist and surgical intensivists for patients with a tracheostomy who were transferred from the surgical intensive care unit (SICU) to the general ward.
-
Methods:
- In this retrospective study, subjects were limited to SICU patients with a tracheostomy who were transferred to the general ward. The study period was divided into a preintervention period (January 1, 2007 to December 31, 2010) and a postintervention period (January 1, 2011 to December 31, 2014), and electronic medical records were used to analyze and compare patient characteristics, clinical outcomes, and readmission to the SICU.
-
Results:
- The analysis included 44 patients in the preintervention group and 96 patients in the postintervention group. Decannulation time (26.7±25.1 vs. 12.1±16.0 days, P=0.003),length of stay in the general ward (70.6±89.1 vs. 40.5±42.2 days, P=0.008), length of total hospital stay (107.5±95.6 vs. 74.7±51.2 days, P=0.009), and readmission rate of SICU decreased due to T-cannula occlusion (58.8% vs. 5.9%, P=0.010).
-
Conclusions:
- Using a systematic approach to tracheostomy care in the general ward led to reduction in decannulation time through professional management, which resulted in a shorter hospital stay. It also lowered SICU readmission by solving problems related to direct T-cannula.
-
Keywords: intensive care units; respiratory care; tracheostomy
INTRODUCTION
A tracheotomy is performed for a variety of reasons including major surgical operations of the head and neck, airway obstruction, prolonged intubation, and aspiration [1,2]. A tracheostomy in the intensive care unit (ICU) is preferred for patients who require prolonged mechanical ventilation or airway clearance due to the presence of secretions and airway obstruction [3]. Furthermore, tracheostomy facilitates suctioning by allowing easy access into the lower airway [4]. As a result, patient safety and comfort improves and patients need less sedation, leading to a shortened duration of ventilator support, and eventually, early discharge from the ICU [5,6]. As tracheostomies increase in the ICU [7], the number of patients who are transferred to the general ward while maintaining tracheostomy is also increasing [8].
Treatment and nursing care of post-ICU patients with a tracheostomy are not easy given the generally inferior monitoring systems and levels of care in the general ward, as well as a lack of sufficient clinical handover between ICU and general ward professionals for the ICU-to-ward transfer of long-term ICU patients [9].
Tracheostomy care in the general ward should be able to closely monitoring and early detection about emergency situation [10]. Possible adverse outcomes, such as obstruction of the T-cannula, underline the importance of specialized knowledge and consistent and regular monitoring for patients with a tracheostomy [11,12].
In the practical context, the ICU-to-ward transfer process can include plans for tracheostomy care and decannulation and a leading role for the relevant ICU nurses in providing nursing care for post-ICU patients with a tracheostomy [13]. This planned approach can boost patient outcomes and improve safety [14]. The purpose of this study was to investigate the effect of managing tracheostomy care in the surgical ward through a systematic approach delivered by team of clinical nurse specialist (CNS) and surgical intensivists.
MATERIALS AND METHODS
Study Subjects
This retrospective study was conducted in the 14-bed surgical ICU (SICU) of a 2,500 bed tertiary center. The study period was divided into the preintervention (January 2007 to December 2010) and the postintervention period (January 2011 to December 2014). Surgical patients with a tracheostomy who were transferred from the SICU to the general ward were included. Patients under the age of 18, who were transferred to the transplantation ward were excluded (Figure 1). This study was approved by the Institutional Review Board of Asan Medical Center (IRB No. 2017-0342).
Methods
Care of patients with tracheostomy during the preintervention period
Before a CNS was available, the patients with a tracheostomies care system operated in three shifts. General ward nursing staff consisted of four teams per ward; nurse to patient ratio of 1:10–15. These nurses did not have experience with tracheostomy patients or training in T-cannula management and nursing.
Care of patients with tracheostomy during the intervention period
To improve patient care, a CNS was hired to develop patient management in collaboration with three intensivists. The involved ICU CNS was a licensed critical care nurse who had worked for 9 years in this institution with responsibilities related to patient management in collaboration with surgical intensivists.
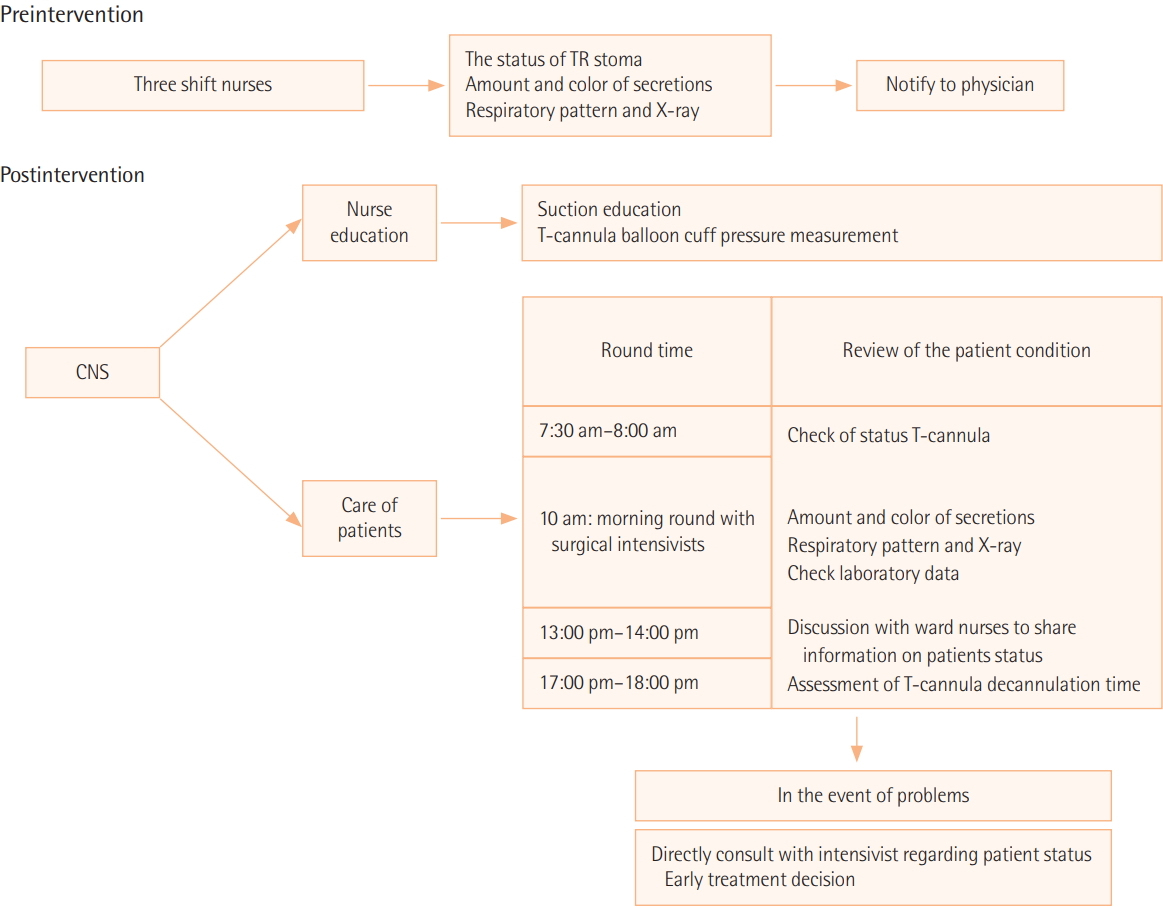
The CNS and intensivists joined the morning rounds for the initial 3 days following transfer to the general ward. Patients requiring follow-up for more than 3 days were followed-up for up to 2 weeks according to the individual’s general condition. From Monday to Friday, the CNS rounded the general ward three times a day to assess patients’ conditions as well as patients’ sputum patterns and respiratory status. She also taught the shift nurses correct suction methodology and how to take a T-cannula balloon cuff pressure measurement. The CNS and intensivists determined that removal of the T-cannula was appropriate by assessing a patient’s range of motion, walking ability, amount of secretions, and ability to self-expectorate. If a problem occurred, the CNS directly contacted an surgical intensivist and collaboratively, the two worked together to resolve the problem in order to maintain coherence and consistency (Figure 2).
Outcome and statistical analysis
The following demographic data were collected: age, sex, initial Acute Physiology and Chronic Health Evaluation (APACHE) II, and Sequential Organ Failure Assessment (SOFA), discharge APACHE II and SOFA, diagnosis, cause of admission into the ICU, route of admission, medical history, average retention time of tracheostomy in SICU, length of stay (LOS) in SICU, total mechanical ventilation day, and last tracheostomy tube change day before transfer to the general ward.
The cardiovascular disease definition of medical history was defined as Angina, Acute myocardial infarction, or a stress induced cardiomyopathy diagnosis. Liver disease was defined as liver cirrhosis or hepatitis. Kidney disease was defined as a patient who is hemodialysis implemented with end-stage renal disease or diagnosed with chronic renal failure. Cerebral disease was defined as a patient with a history of stroke.
Primary clinical outcomes for both pre- and postintervention groups were tracheostomy tube change in the general ward and time to decannulation, whereas secondary outcomes were LOS of general ward, LOS of hospital, hospital mortality, and readmission to the SICU.
Categorical data were analyzed using the Fisher exact tests or Pearson chi-square tests, and continuous variables were analyzed using the Student t-test and Mann-Whitney U-test for normally and non-normally distributed data. All statistical analyses were performed using the SPSS version 11.0 (SPSS Inc., Chicago, IL, USA). A P-value of less than 0.05 was considered statistically significant.
RESULTS
Patient Characteristics
The total number of tracheostomy patients in the SICU preintervention group (from 2007 to 2011) was 151. Forty-four of every 100 patients with a tracheostomy were transferred to the general ward, except 47 patients who died in the SICU and four patients who were transferred to other hospitals. The total number of tracheostomy patients in the SICU postintervention (from 2011 to 2014) was 264. Ninety-six out of every 202 with a tracheostomy were transferred to the general ward, except 54 patients who died in the SICU and eight patients who were transferred to other hospitals (Figure 1). Male patients outnumbered female patients in both groups, and the mean age was 65.3±13.6 years and 63.4±17.9 years in the preand postintervention groups, respectively, showing no significant difference. There was no significant difference in APACHE II scores at initial SICU admission (P=0.350) and at SICU discharge (P=0.370) between the two groups. Trauma was the most common diagnosis at initial SICU admission in the two groups (31.8% vs. 31.3%), followed by postsurgery care. However, no difference was shown between the groups regarding admission diagnosis. The timing of tracheostomy after SICU admission was similar (9.4±5.9 days and 8.7±5.5 days preand postintervention, respectively). There was no difference in length of SICU stay or duration of mechanical ventilation between the groups. Mean length of SICU stay was 26.0±15.9 and 28.3±21.3 days pre- and postintervention, respectively. The average tracheostomy tube replacement time at SICU discharge was 3.4±3.9 and 4.4±3.9 days pre- and postintervention, respectively (Table 1).
Clinical Outcomes Preintervention and Postintervention
The time to the first tracheostomy tube change in the general ward was 6.1±6.1 and 2.3±3.1 days before and after intervention, respectively, showing a reduction of almost 4 days (P<0.000). Although there was no difference between the groups with respect to the number of patients planned for decannulation (52.3% vs. 56.2%, P=0.590), time to decannulation was decreased from 26.7±25.1 days before intervention to 12.1±16.0 days after intervention, showing a reduction of almost 14 days (P=0.003).
The LOS in the general ward was decreased from 70.6±89.1 days before intervention to 40.5±42.2 days after intervention, resulting in a reduction of about 30 days (P=0.008). The length of total hospital stay also significantly decreased (107.5±95.6 vs. 74.7±51.2, P=0.009). There was no difference in mortality rate (4.5% vs. 5.2%, P=0.867) between the two groups, while the ICU readmission rate (45.5% vs. 23.9%, P=0.009) was significantly reduced. For reasons for ICU readmission, respiratory problems were the most common (85.0% vs. 73.9%) in the two groups (Table 2).
Reasons for SICU Readmission Due to Respiratory Problems
Further analysis of respiratory problems revealed that T-cannula-related problems significantly decreased (58.8% vs. 11.8%, P=0.010). However, respiratory infection complications, such as increase of secretions (5.9% vs. 23.5%) and aggravated pneumonia (11.8% vs. 23.5%) were not decreased (P=0.034) (Table 3).
DISCUSSION
In this study, we investigated the effect of managing tracheostomy care in the surgical ward through a systematic approach delivered by team of CNS and surgical intensivists. Despite the increase in the number of tracheostomy patients in the general ward after the postintervention showed reduction in time to decannulation, decreased LOS general ward and hospitalization and readmission SICU.
The number of SICU patients with tracheostomies transferred to the general ward increased from 44 before intervention to 96 after intervention. The difference can be attributed to the increase in the number of patients who underwent tracheostomy after initial admission to the SICU. The reason for the increased incidence of tracheotomy is the increasing trend of patients who need to use high-tech special devices due to the development of treatment along with the increasing aging population [5]. Many patients keep the tracheostomy in situ while being transferred to the general ward. This confirms that the physiological risk factors for respiratory failure are associated with the aging process [12].
Trauma patients constituted the largest proportion of all post-SICU patients with a tracheostomy. This finding is consistent with a previous study in which the patients who had an altered level of consciousness resulting from severe traumatic brain injury required less sedation after tracheostomy because they did not have physical comorbidities, enabling them to have a shorter duration of mechanical ventilation and quicker transfer to the general ward than those with comorbidities [10].
After postintervention tracheostomy care was provided, the time to first tracheostomy tube change was reduced in the general ward. This finding is likely attributable to the early detection of problems associated with the introduction of the suctioning catheter and immediate change of the respective tracheostomy tube while the CNS reviewed the patient’s conditions during ward rounds that were conducted three times per day. In addition, the status of the tracheostomy stoma and respiratory patterns were closely checked. Such an early tracheostomy tube replacement can significantly reduce SICU readmission caused by tracheostomy tube obstruction, which was most prevalent before intervention.
The blockage of the tracheostomy tube is mostly due to secretions and aspiration. In other words, oxygen is not properly heated and humidified while passing through the upper airway, and the dry airflow directly enters the tube and leaves mucous membranes dry, which induces deep mucus production [15]. Hooper [13] recommended the use of a saline nebulizer at intervals of 2–4 hours when mucus is thick and dry. In this study, an all-purpose nebulizer or a nebulizer was actively used for patients who were considered at risk of tracheostomy tube obstruction.
In addition, the number of patients for whom decannulation was planned showed no significant difference during the same period. Decannulation can be considered when patients demonstrate stable respiratory patterns, effective cough, and the ability to protect their own airway. Therefore, it is important to assess patients on a regular basis and take a planned approach in order to improve patient outcomes and safety [10]. In this study, it was removed if it was deemed possible to remove the T-cannula through assessment of the range of walking and motion, amount of secretions, and possibility of self expectoration.
The LOS in the general ward significantly decreased from 70.6±89.1 days preintervention to 40.5±42.2 days postintervention. A further analysis revealed that the LOS in the ward was significantly reduced, regardless of whether decannulation was performed. The shortened LOS in the ward for post-SICU patients with a tracheostomy can be explained by the assumption that these patients might have required a tracheostomy for a longer time because of their altered level of consciousness and difficulties in sputum expectoration, and they might have been prematurely transferred to a long-term care facility, such as a convalescent hospital. A reduction in the LOS in the general ward eventually shortened the length of the total hospital stay. This finding supports a previous study claiming that intensive care of patients with tracheostomy can reduce length of hospital stay and other serious problems [16].
As the timing of decannulation was planned through regular monitoring performed by the CNS, the decannulation time decreased from 26.7±25.1 days preintervention to 12.1±16.0 days postintervention. This finding is consistent with a previous study reporting a shorter decannulation time under a systematic approach [10].
In many literatures, the mortality rate of patients with tracheostomy patients in the ward was reported to be high [7,17]. This study showed no difference in the mortality rate pre- and post-tracheostomy tube management. Based on the published literature, the mortality rate should be high after postintervention group. It can be explained that there was no difference in the mortality rate before and after the incision management through proper management of the tracheotomy patient.
Apart from tracheostomy tube obstruction, the occurrence of other respiratory problems, such as large amounts of secretion and aspiration and septic shock, was not significantly different between the pre- and postintervention groups. In this study, tracheostomy patient care was not maintained steadily during the weekend, resulting in insufficient continuity of tracheostomy patient care. Furthermore, three rounds a day made it difficult to reduce pneumonia or respiratory infections. In the study of de Mestral et al. [10], a systematic approach succeeded in managing tracheostomy care and reducing tracheostomy-related emergencies, but did not curb respiratory infection, unplanned extubation, and bleeding. Similarly, this study also found no significant difference in the occurrence of respiratory problems other than tracheostomy tube obstruction between the pre- and postintervention groups.
In conclusion, CNS with surgical intensivist-led tracheostomy care had a positive effect about lowered SICU readmission by early solving problem such as obstruction of the tracheostomy. Also as decannulation time was accelerated, LOS in the general ward and total hospital stay were shortened. but our study shows that constant 24 hours systematic monitoring and intensive management are necessary. In order to provide such care, we suggest the establishment of a sub-ICU in which care can be continuous for intensive care transfer patients with tracheostomies.
KEY MESSAGES
▪ The management of tracheostomy patients in general wards shorter decannulation time under systematic approach.
▪ The management of tracheotomy patients in general wards lowers the readmission rate of surgical intensive care unit associated with tracheotomy tube problems.
▪ In order to manage problems such as respiratory infections, it is necessary to establish a sub-intensive care unit that can be managed continuously and steadily.
NOTES
-
No potential conflict of interest relevant to this article was reported.
Figure 1.Flow diagram of preintervention and postintervention patient enrollment. SICU: surgical intensive care unit; GW: general ward.

Figure 2.Comparison of pre- and postintervention tracheostomy care. TR: tracheostomy; CNS: clinical nurse specialist.

Table 1.Patients’ baseline characteristics (n=140)
|
Characteristics |
Preintervention group (n=44) |
Postintervention group (n=96) |
P-value |
|
Sex |
|
|
0.151 |
|
Male |
36 (81.8) |
66 (68.8) |
|
|
Female |
8 (18.2) |
30 (31.2) |
|
|
Age (yr) |
65.3±13.6 |
63.4±17.9 |
0.517 |
|
At ICU admission |
|
|
|
|
APACHE II score |
16.5±7.0 |
17.7±7.3 |
0.350 |
|
SOFA score |
5.9±2.7 |
5.4±3.1 |
0.401 |
|
At discharge from ICU |
|
|
|
|
APACHE II score |
13.5±6.5 |
16.4±6.8 |
0.370 |
|
SOFA score |
2.0±1.6 |
2.2±1.9 |
0.402 |
|
Discharge ICU GCS |
12.5±3.1 |
14.3±1.1 |
0.780 |
|
Diagnosis |
|
|
0.310 |
|
Vascular disease |
6 (13.6) |
6 (6.3) |
|
|
Cancer |
11 (25.0) |
17 (17.7) |
|
|
Trauma |
14 (31.8) |
30 (31.3) |
|
|
Bowel disease |
11 (25.0) |
33 (4.4) |
|
|
Others |
2 (4.6) |
10 (10.4) |
|
|
Cause of admission in ICU |
|
|
0.152 |
|
Postoperative care |
15 (34.1) |
30 (31.3) |
|
|
Septic shock |
4 (9.1) |
10 (10.4) |
|
|
Trauma |
13 (29.5) |
30 (31.3) |
|
|
Bleeding |
1 (2.3) |
10 (10.4) |
|
|
Respiratory disorder |
11 (25.0) |
13 (13.5) |
|
|
Heart failure |
0 |
3 (3.1) |
|
|
Route of admission |
|
|
0.569 |
|
Emergency room |
16 (37.2) |
27 (62.8) |
|
|
Operation room |
17 (27.4) |
45 (46.9) |
|
|
General ward |
11 (31.4) |
24 (25.0) |
|
|
Medical history |
26 (59.1) |
51 (53.1) |
0.585 |
|
HTN |
17 (41.5) |
38 (40.4) |
0.989 |
|
DM |
14 (34.1) |
28 (29.8) |
|
|
COPD |
2 (4.9) |
4 (4.3) |
|
|
Cardiovascular disease |
3 (7.3) |
8 (8.5) |
|
|
Liver disease |
1 (2.4) |
5 (5.3) |
|
|
Kidney disease |
1 (2.4) |
4 (4.3) |
|
|
Cerebral disease |
3 (2.1) |
7 (7.4) |
|
|
Average retention time of tracheostomy in SICU |
9.4±5.9 |
8.7±5.5 |
0.889 |
|
Length of stay in SICU |
26.0±15.9 |
28.3±21.3 |
0.486 |
|
Total mechanical ventilation day |
22.3±16.3 |
26.9±20.3 |
0.181 |
|
Last tracheostomy tube change day before transfer to general ward |
3.4±3.9 |
4.4±3.9 |
0.835 |
Table 2.Clinical outcomes preintervention and postintervention (n=140)
|
Characteristics |
Preinterven- tion group (n=44) |
Postinterven- tion group (n=96) |
P-value |
|
Time to first tracheostomy tube change in general ward |
6.1±6.1 |
2.3±3.1 |
<0.000 |
|
Patients who underwent successful decannulation |
23 (52.3) |
54 (56.2) |
0.590 |
|
Time to decannulation (day) |
26.7±25.1 |
12.1±16.0 |
0.003 |
|
General ward LOS (day) |
70.6±89.1 |
40.5±42.2 |
0.008 |
|
Hospital LOS (day) |
107.5±95.6 |
74.7±51.2 |
0.009 |
|
Mortality |
2 (4.5) |
5 (5.2) |
0.867 |
|
Readmission to ICU |
20 (45.5) |
23 (23.9) |
0.009 |
|
Time to readmission to ICU |
10.9±27.2 |
8.6±8.7 |
0.705 |
|
Reason for ICU |
|
|
0.405 |
|
Respiratory problem |
17 (85.0) |
17 (73.9) |
|
|
Sceptic shock |
3 (15.0) |
4 (17.4) |
|
|
Bleeding, others |
0 |
2 (8.7) |
|
Table 3.Readmission to SICU due to respiratory problems (n=34)
|
Characteristics |
Preinterven- tion group (n=17) |
Postinterven- tion group (n=17) |
P-value |
|
T-cannula-related problem |
|
|
0.010 |
|
T-cannula occlusion |
10 (58.8) |
1 (5.9) |
|
|
T-cannula dislocation |
0 |
1 (5.9) |
|
|
Respiratory infection |
|
|
0.034 |
|
Aspiration |
4 (23.5) |
5 (29.4) |
|
|
Increased amount of secretion |
1 (5.9) |
4 (23.5) |
|
|
Atelectasis |
0 |
2 (11.8) |
|
|
Aggravated pneumonia |
2 (11.8) |
4 (23.5) |
|
References
- 1. Casserly P, Lang E, Fenton JE, Walsh M. Assessment of healthcare professionals’ knowledge of managing emergency complications in patients with a tracheostomy. Br J Anaesth 2007;99:380-3.ArticlePubMedPDF
- 2. Durbin CG Jr. Tracheostomy: why, when, and how? Respir Care 2010;55:1056-68.PubMed
- 3. Cameron M, Corner A, Diba A, Hankins M. Development of a tracheostomy scoring system to guide airway management after major head and neck surgery. Int J Oral Maxillofac Surg 2009;38:846-9.ArticlePubMed
- 4. Stelfox HT, Crimi C, Berra L, Noto A, Schmidt U, Bigatello LM, et al. Determinants of tracheostomy decannulation: an international survey. Crit Care 2008;12:R26. ArticlePubMedPMC
- 5. Engoren M, Arslanian-Engoren C, Fenn-Buderer N. Hospital and long-term outcome after tracheostomy for respiratory failure. Chest 2004;125:220-7.ArticlePubMed
- 6. Norwood MG, Spiers P, Bailiss J, Sayers RD. Evaluation of the role of a specialist tracheostomy service: from critical care to outreach and beyond. Postgrad Med J 2004;80:478-80.ArticlePubMedPMC
- 7. Paul F. Tracheostomy care and management in general wards and community settings: literature review. Nurs Crit Care 2010;15:76-85.ArticlePubMed
- 8. Ball C. Ensuring a successful discharge from intensive care. Intensive Crit Care Nurs 2005;21:1-4.ArticlePubMed
- 9. Russell S. Continuity of care after discharge from ICU. Prof Nurse 2000;15:497-500.PubMed
- 10. de Mestral C, Iqbal S, Fong N, LeBlanc J, Fata P, Razek T, et al. Impact of a specialized multidisciplinary tracheostomy team on tracheostomy care in critically ill patients. Can J Surg 2011;54:167-72.ArticlePubMedPMC
- 11. Lewis T, Oliver G. Improving tracheostomy care for ward patients. Nurs Stand 2005;19:33-7.Article
- 12. Docherty B, Bench S. Tracheostomy management for patients in general ward settings. Prof Nurse 2002;18:100-4.PubMed
- 13. Hooper M. Nursing care of the patient with a tracheostomy. Nurs Stand 1996;10:40-3.Article
- 14. Tamburri LM. Care of the patient with a tracheostomy. Orthop Nurs 2000;19:49-58.Article
- 15. Buglass E. Tracheostomy care: tracheal suctioning and humidification. Br J Nurs 1999;8:500-4.ArticlePubMed
- 16. Speed L, Harding KE. Tracheostomy teams reduce total tracheostomy time and increase speaking valve use: a systematic review and meta-analysis. J Crit Care 2013;28:216.e1-10. ArticlePubMed
- 17. Fernandez R, Bacelar N, Hernandez G, Tubau I, Baigorri F, Gili G, et al. Ward mortality in patients discharged from the ICU with tracheostomy may depend on patient’s vulnerability. Intensive Care Med 2008;34:1878-82.ArticlePubMed
Citations
Citations to this article as recorded by

- Quality tracheotomy care can be maintained for non‐COVID patients during the COVID‐19 pandemic
Jacqueline Tucker, Nicole Ruszkay, Neerav Goyal, John P. Gniady, David Goldenberg
Laryngoscope Investigative Otolaryngology.2022; 7(5): 1337. CrossRef - Global Tracheostomy Collaborative: data-driven improvements in patient safety through multidisciplinary teamwork, standardisation, education, and patient partnership
Michael J. Brenner, Vinciya Pandian, Carly E. Milliren, Dionne A. Graham, Charissa Zaga, Linda L. Morris, Joshua R. Bedwell, Preety Das, Hannah Zhu, John Lee Y. Allen, Alon Peltz, Kimberly Chin, Bradley A. Schiff, Diane M. Randall, Chloe Swords, Darrin Fr
British Journal of Anaesthesia.2020; 125(1): e104. CrossRef
 , Younghwan Kim2
, Younghwan Kim2 , Kyuhyouck Kyoung3
, Kyuhyouck Kyoung3 , Minae Keum3
, Minae Keum3 , Taehyun Kim2
, Taehyun Kim2 , Dae seong Ma4
, Dae seong Ma4 , Suk-Kyung Hong5
, Suk-Kyung Hong5









 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite