Articles
- Page Path
- HOME > Acute Crit Care > Forthcoming articles > Article
-
Case Report
Cardiology Successful neural modulation of bedside modified thoracic epidural anesthesia for ventricular tachycardia electrical storm -
Ki-Woon Kang

-
DOI: https://doi.org/10.4266/acc.2021.01683
Published online: May 31, 2022
Division of Cardiology, Chung-Ang University Hospital, Chung-Ang University College of Medicine, Seoul, Korea
- Corresponding author: Ki-Woon Kang Division of Cardiology, Chung-Ang University Hospital, 102 Heukseok-ro, Dongjak-gu, Seoul 06973, Korea Tel: +82-2-6299-2871; Fax: +82-2-6299-2871, E-mail: kwkang0115@gmail.com
• Received: November 17, 2021 • Revised: March 3, 2022 • Accepted: March 7, 2022
Copyright © 2022 The Korean Society of Critical Care Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 1,810 Views
- 35 Download
- 1 Crossref
Abstract
- Ventricular tachycardia (VT)/ventricular fibrillation (VF) storm can be hemodynamically compromising and life-threatening. Management of medically refractory VT/VF storm is challenging in the intensive care unit. A 38-year-old male patient was diagnosed with non-ischemic heart failure and acute kidney injury with documented frequent premature ventricular contraction with QT prolongation after recurrent VT/VF. Even though the patient was intubated with sedatives and had taken more than two anti-arrhythmic drugs with external recurrent defibrillation at bedside, the electrical storm persisted for several hours. However, medically refractory VT/VF storm can be successfully and rapidly terminated with a modified thoracic epidural anesthesia at bedside. This case demonstrates that a bedside thoracic epidural anesthesia can be an effective non-pharmacological option to treat medically refractory VT/VF storm in the intensive care unit.
CASE REPORT
DISCUSSION
Figure 1.(A) Rhythm strip shows a prolonged QT interval with a giant T-wave inversion (blue dotted line) and sudden initiation of ventricular tachycardia. Black arrow indicates first premature ventricular beat inducing ventricular tachycardia. (B) Rhythm strip shows sustained ventricular fibrillation degeneration in the setting of a long QT interval. (C) Rhythm strip shows that the incessant ventricular tachycardia/fibrillation was promptly terminated (asterisk) and restored to a sinus rhythm (blue dotted line) after the thoracic epidural anesthesia. ECG: electrocardiogram.
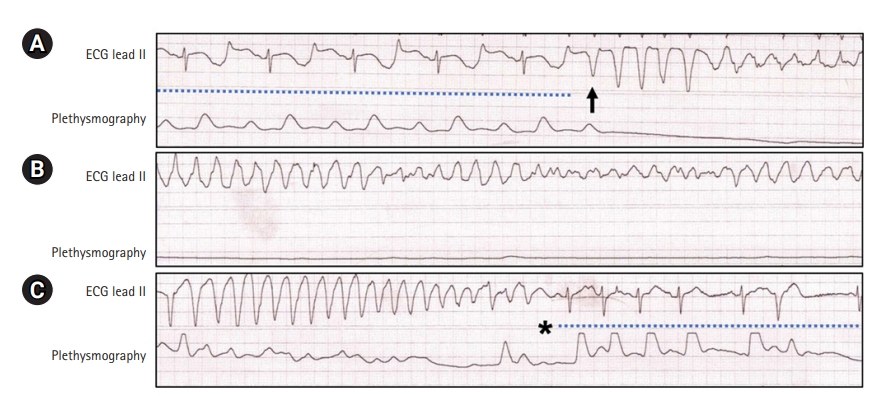

Figure 2.(A) Intubation tube (black arrow), right jugular vein sheath and defibrillation patch (asterisk) linear thoracic epidural catheter (white arrows). (B) Anatomical position of 18-G Tuohy needle with loss of resistance technique.
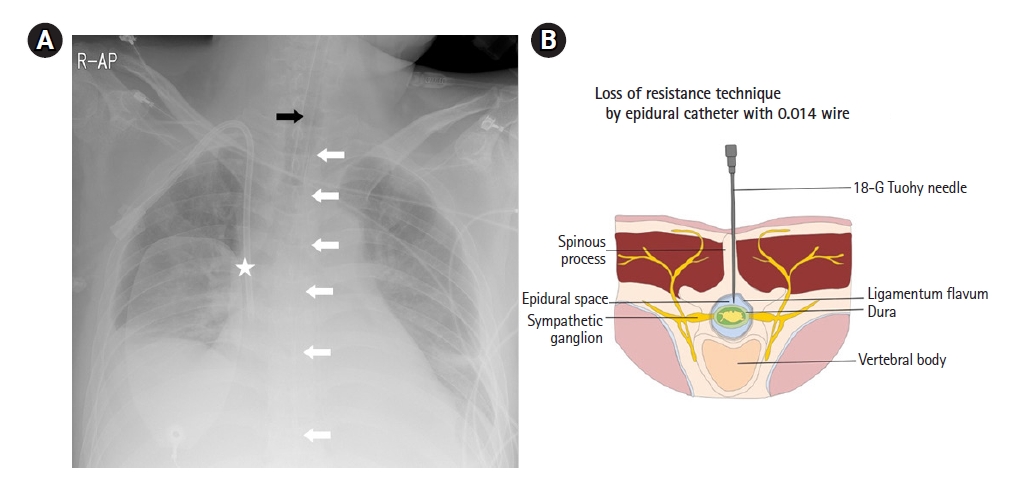

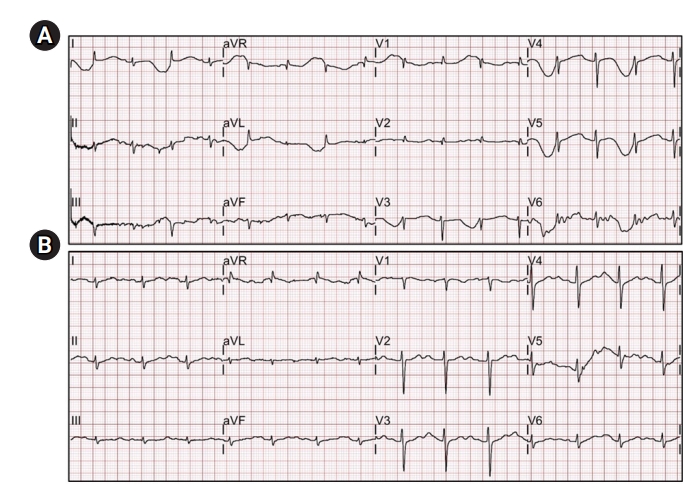
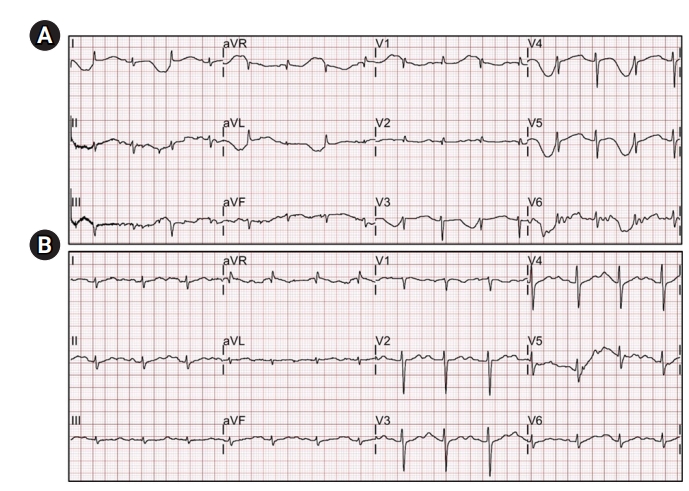
Figure 3.(A) A 12-lead electrocardiogram (ECG) shows a prolonged QT interval with a giant T-wave inversion before initiation of ventricular tachycardia at the period of the blue dotted line in Figure 1A. (B) A 12-lead ECG shows normalized QT prolongation with T-wave inversion after the thoracic epidural anesthesia at the period of the blue dotted line in Figure 1C. aVR: augmented vector right; aVL: augmented vector left; aVF: augmented vector foot.

- 1. Al-Khatib SM, Stevenson WG, Ackerman MJ, Bryant WJ, Callans DJ, Curtis AB, et al. 2017 AHA/ACC/HRS guideline for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. Circulation 2018;138:e272-391.ArticlePubMed
- 2. Do DH, Bradfield J, Ajijola OA, Vaseghi M, Le J, Rahman S, et al. Thoracic epidural anesthesia can be effective for the short-term management of ventricular tachycardia storm. J Am Heart Assoc 2017;6:e007080. ArticlePubMedPMC
- 3. Kotake Y, Kurita T, Akaiwa Y, Yasuoka R, Motoki K, Kobuke K, et al. Intravenous amiodarone homogeneously prolongs ventricular repolarization in patients with life-threatening ventricular tachyarrhythmia. J Cardiol 2015;66:161-7.ArticlePubMed
- 4. Yonai R, Kawabata M, Maeda S, Kawashima T, Tsuda Y, Nakasone T, et al. Torsade de pointes induced by intravenous amiodarone therapy accompanied by marked augmentation of the transmural dispersion of repolarization in a patient with tachycardia-induced-cardiomyopathy. Ann Noninvasive Electrocardiol 2021;26:e12810. ArticlePubMedPMCPDF
- 5. Meng L, Tseng CH, Shivkumar K, Ajijola O. Efficacy of stellate ganglion anesthesiaade in managing electrical storm: a systematic review. JACC Clin Electrophysiol 2017;3:942-9.ArticlePubMedPMC
- 6. Bradfield JS, Ajijola OA, Vaseghi M, Shivkumar K. Mechanisms and management of refractory ventricular arrhythmias in the age of autonomic modulation. Heart Rhythm 2018;15:1252-60.ArticlePubMed
- 7. Howard-Quijano K, Takamiya T, Dale EA, Yamakawa K, Zhou W, Buckley U, et al. Effect of thoracic epidural anesthesia on ventricular excitability in a porcine model. Anesthesiology 2017;126:1096-106.ArticlePubMedPDF
- 8. Ajijola OA, Lellouche N, Bourke T, Tung R, Ahn S, Mahajan A, et al. Bilateral cardiac sympathetic denervation for the management of electrical storm. J Am Coll Cardiol 2012;59:91-2.ArticlePubMedPMC
- 9. Estes EH Jr, Izlar HL Jr. Recurrent ventricular tachycardia: a case successfully treated by bilateral cardiac sympathectomy. Am J Med 1961;31:493-7.ArticlePubMed
- 10. Wink J, Veering BT, Aarts LP, Wouters PF. Effects of thoracic epidural anesthesia on neuronal cardiac regulation and cardiac function. Anesthesiology 2019;130:472-91.ArticlePubMedPDF
- 11. Kang XH, Bao FP, Xiong XX, Li M, Jin TT, Shao J, et al. Major complications of epidural anesthesia: a prospective study of 5083 cases at a single hospital. Acta Anaesthesiol Scand 2014;58:858-66.ArticlePubMed
References
Figure & Data
References
Citations
Citations to this article as recorded by 

- Continuous stellate ganglion block for ventricular arrhythmias: case series, systematic review, and differences from thoracic epidural anaesthesia
Veronica Dusi, Filippo Angelini, Enrico Baldi, Antonio Toscano, Carol Gravinese, Simone Frea, Sara Compagnoni, Arianna Morena, Andrea Saglietto, Eleonora Balzani, Matteo Giunta, Andrea Costamagna, Mauro Rinaldi, Anna Chiara Trompeo, Roberto Rordorf, Matte
Europace.2024;[Epub] CrossRef

 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite