Abstract
- Portable chest radiography is a valuable tool in the intensive care unit. However, the supine position causes superposition of anatomical structures resulting in less reliable detection of certain abnormalities. Recently, a portable digital tomosynthesis (pDTS) prototype with a modified motorized X-ray device was developed. We aimed to compare the diagnostic value of pDTS to standard bedside chest radiography in the diagnosis of a posterior pneumothorax. A modified motorized X-ray device was developed to perform 15 radiographic projections while translating the X-ray tube 25 cm (10 cm ramp up and 15 cm during X-ray exposure) with a total radiation dose of 0.54 mSv. This new technique of pDTS was performed in addition to standard bedside chest X-ray in a patient with a confirmed posterior hydropneumothorax. The images were compared with the standard bedside chest X-ray and computed tomography (CT) images by two experienced radiologists. The posterior hydropneumothorax previously identified with CT was visible on tomosynthesis images but not with standard bedside imaging. Combining the digital tomosynthesis technique with the portable X-ray machine could increase the diagnostic value of bedside chest radiography for the diagnosis of posterior pneumothoraces while avoiding intrahospital transport and limiting radiation exposure compared to CT.
-
Keywords: bedside chest X-ray; digital tomosynthesis; intensive care unit; posterior pneumothorax
Pneumothorax is a common problem in adult intensive care unit (ICU) patients with a prevalence of 4%–15% in mechanically ventilated patients [1], and up to 50% in patients following chest trauma [2]. Currently, computed tomography (CT)-scan is the gold standard for both the diagnosis and assessing the size of the pneumothorax [3]. Recently, portable digital tomosynthesis (pDTS) prototype with a modified motorized X-ray device was developed [4]. pDTS is a technique where several low dose X-ray images are acquired with a motorized X-ray source which moves relative to a stationary detector. Subsequently, reconstruction algorithms are used to compute coronal section images through the area of interest. This technique may be able to improve the diagnostic value of bedside chest radiography due to its ability to distinguish overlapping anatomical structures. Chest digital tomosynthesis is a technique already available on a wall mounted flat panel or X-ray table, however, there is currently no pDTS available on the market [5].
We describe a case that highlights its potential in critically ill patients. This study was approved by our local Institutional Review Board (IRB No. 143202043138) and all patients or designated proxies provided written informed consent. Authors with no ties to Agfa Radiology Solutions had unrestricted control over the data during the study.
CASE REPORT
A 62-year-old man was admitted to the ICU following respiratory failure due to coronavirus disease 2019 (COVID-19) pneumonia. His stay was further complicated by several ventilator acquired pneumonias and the requirement of venovenous extracorporeal membrane oxygenation. Due to respiratory deterioration on day 41 of hospital admission a CT thorax was performed which initially showed subcutaneous emphysema and a pneumomediastinum without evidence of a pneumothorax (Figure 1A). Respectively, 2 and 7 days later, a pneumothorax at the left apex as well as at the right apex was visualized on a standard bedside chest X-ray for which a chest drain was placed (Figure 1B-E). Twelve days after the initial CT scan a new CT scan was performed to re-evaluate the extent of the pneumothoraces after drain insertion. This showed an additional posterobasal hydropneumothorax on the right which was not visible on standard bedside chest X-ray (Figure 1F). Subsequently, an additional chest drain was inserted. Analysis of the fluid suggested an empyema for which antibiotics were initiated.
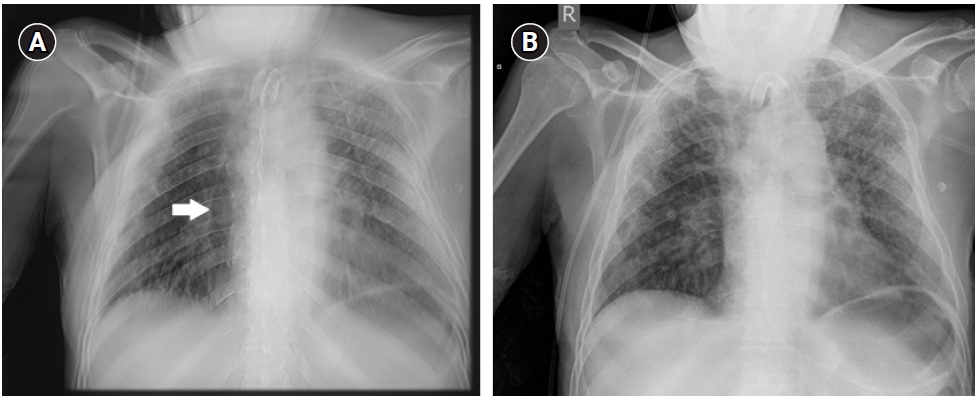
After the acute phase, on day 151 since admission, a portable DTS acquisition was performed in addition to the standard bed-side chest radiography with a prototype device (Agfa Radiology Solutions). Fifteen X-ray projections were made while translating the X-ray tube 25 cm with a synchronized motorized system (10 cm ramp up and 15 cm during X-ray exposure) with a total acquisition time of about 3.2 seconds. Subsequently images were reconstructed using the simultaneous iterative reconstruction technique (SIRT) algorithm using 25 iterations. The estimated effective radiation dose of the pDTS acquisition was 0.54 mSv (in comparison to a typical radiation dose of 0,1 mSv in standard chest radiography, and 6.2 mSv for chest CT) [6]. A radiological comparison was made between the pDTS images and the standard bedside chest X-ray by two experienced chest radiologists. A posterior (hydro)pneumothorax which had previously been identified with CT thorax appeared while scrolling through the tomosynthesis images (Figure 2A) but was not visible on the standard bedside radiography imaging (Figure 2B).
DISCUSSION
Portable chest radiography is a valuable tool frequently used in ICU, especially when the condition of the patient deteriorates. However, the supine position anteroposterior exam in a bedbound ICU patient with suboptimal positioning causes superposition of anatomical structures resulting in less reliable detection of certain abnormalities, such as a pneumothorax [7]. The presented case describes the potential diagnostic benefit of the pDTS technique compared to the standard portable chest X-ray. The combination of digital tomosynthesis technique with the already widely used portable X-ray machine could increase the diagnostic value of portable chest radiography in ICU as is presented in this case.
Ultrasound is a useful bedside radiological technique which, in the diagnosis of pneumothorax, has been shown to have a higher sensitivity and similar specificity compared to standard chest X-ray. However, the accuracy of ultrasound in the diagnosis of pneumothorax is operator-dependent and requires a critical care ultrasound-trained physician [8].
CT scan is currently the gold standard for the diagnosis and assessing the size of a pneumothorax. CT scan still has an advantage compared to pDTS with regards to assessing the size of a pneumothorax, as further studies are still required to assess the calibration of pDTS as well as the characterization of error margins of measurements. However, there are two major disadvantages of CT scan compared to pDTS. First, in order to perform a CT scan, the patient requires an intrahospital transport. This transport is associated with numerous risks and complications (up to 60%) [9]. Portable CT scanners, if available, are expensive and would require logistical adaptations to be utilized in the ICU setting. pDTS can be readily performed bedside, eliminating the risks associated with intrahospital transport of the patient, in turn also decreasing the risk of virus transmission in the current COVID-19 pandemic.
Secondly, pDTS is associated with a much lower radiation dose (0.54 mSv) than a chest CT scan (6.2 mSv) [6]. ICU patients have an important radiation exposure due to repetitive thorax radiography and CT scans [10]. Following the ALARA principle (as low as reasonably achievable), it is appropriate to limit radiation exposure in ICU patients. Using pDTS would reduce the cumulative radiation exposure if CT scan could be avoided.
Although the technique seems promising, further research is needed. In the ICU setting imaging is subject to respiration motion artefact. The application of a motion correction algorithm could therefore further improve image quality, however, this is subject to further research. Furthermore, it is necessary to evaluate the sensitivity and specificity of this new technology. In order to do so, the comparison with CT scan, classic chest radiography and ultrasonography must be made in critically ill patients to assess the place of pDTS for the diagnosis of pneumothorax in the ICU setting.
NOTES
-
CONFLICT OF INTEREST
Johan De Mey is a member of advisory board Agfa NV, Radiology Solutions, Mortsel, Belgium and Vincent Van Nieuwenhove and Jeroen Cant are employees of Agfa NV, Radiology Solutions, Mortsel, Belgium. No other potential conflicts of interest relevant to this article were reported.
-
AUTHOR CONTRIBUTIONS
Conceptualization: JDM, JJ, VVN, JC. Data curation: JJ. Formal analysis: JDM, JJ. Methodology: JDM, JJ, VVN, JC. Project administration: JDM. Writing–original draft: SW. Writing–review & editing: JJ, NB, JDM.
Figure 1.(A) Computed tomography (CT) thorax on day 41 of admission showing subcutaneous emphysema and a pneumomediastinum (arrow). (B) Standard bedside chest X-ray. Arrow, pneumothorax at the left apex. (C) Standard bedside chest X-ray after drain insertion (left). Arrow, resolution of the pneumothorax at the left apex with drain in situ. (D) Standard bedside chest X-ray: pneumothorax at the right apex (arrow). (E) Standard bedside chest X-ray after drain insertion (right). Arrow, resolution of the pneumothorax at the right apex with drain in situ.
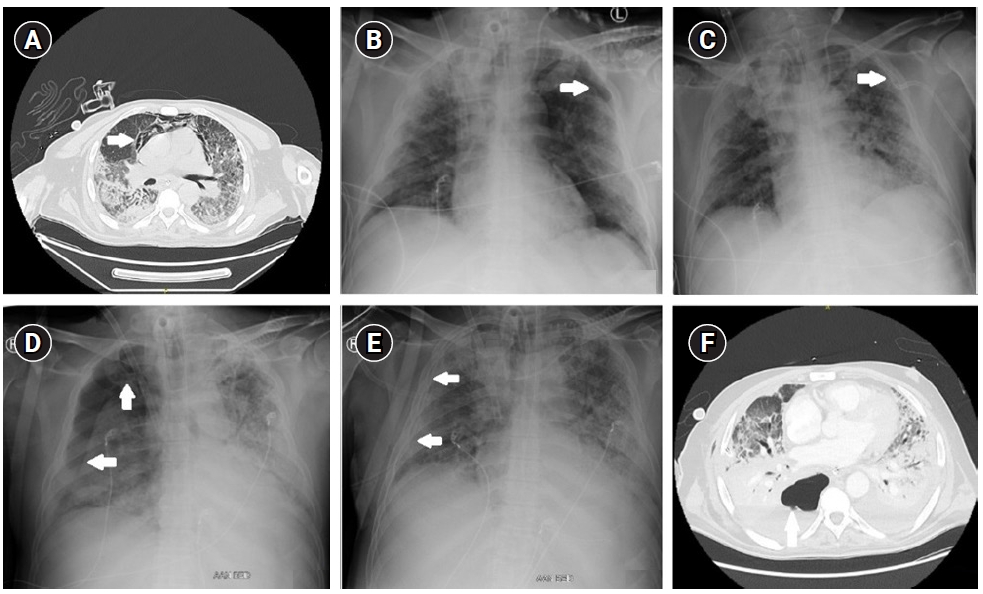
Figure 2.(A) Bedside portable digital tomosynthesis image showing a posterior pneumothorax on the right thorax (arrow). (B) Standard bedside chest radiography: no pneumothorax visible.
References
- 1. Strange C. Pleural complications in the intensive care unit. Clin Chest Med 1999;20:317-27.ArticlePubMed
- 2. Wilson H, Ellsmere J, Tallon J, Kirkpatrick A. Occult pneumothorax in the blunt trauma patient: tube thoracostomy or observation? Injury 2009;40:928-31.ArticlePubMed
- 3. Kelly AM, Weldon D, Tsang AY, Graham CA. Comparison between two methods for estimating pneumothorax size from chest X-rays. Respir Med 2006;100:1356-9.ArticlePubMed
- 4. Cant J, Snoeckx A, Behiels G, Parizel PM, Sijbers J. Can portable tomosynthesis improve the diagnostic value of bedside chest X-ray in the intensive care unit? A proof of concept study. Eur Radiol Exp 2017;1:20. ArticlePubMedPMC
- 5. Dobbins JT 3rd, McAdams HP, Godfrey DJ, Li CM. Digital tomosynthesis of the chest. J Thorac Imaging 2008;23:86-92.ArticlePubMed
- 6. Mettler FA Jr, Mahesh M, Bhargavan-Chatfield M, Chambers CE, Elee CE, Frush DP, et al. Patient exposure from radiologic and nuclear medicine procedures in the united states: procedure volume and effective dose for the period 2006-2016. Radiology 2020;May;295:418-27.ArticlePubMed
- 7. Kollef MH. Risk factors for the misdiagnosis of pneumothorax in the intensive care unit. Crit Care Med 1991;19:906-10.ArticlePubMed
- 8. Ding W, Shen Y, Yang J, He X, Zhang M. Diagnosis of pneumothorax by radiography and ultrasonography: a meta-analysis. Chest 2011;140:859-66.ArticlePubMed
- 9. Fanara B, Manzon C, Barbot O, Desmettre T, Capellier G. Recommendations for the intra-hospital transport of critically ill patients. Crit Care 2010;14:R87. ArticlePubMedPMC
- 10. Krishnan S, Moghekar A, Duggal A, Yella J, Narechania S, Ramachandran V, et al. Radiation exposure in the medical ICU: predictors and characteristics. Chest 2018;153:1160-8.ArticlePubMed
Citations
Citations to this article as recorded by

 , Nico Buls2
, Nico Buls2 , Johan De Mey2
, Johan De Mey2 , Vincent Van Nieuwenhove3
, Vincent Van Nieuwenhove3 , Jeroen Cant3
, Jeroen Cant3 , Joop Jonckheer4
, Joop Jonckheer4








 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite



