Abstract
-
Background
- Arrhythmias are known complication after surgery for congenital heart disease (CHD). This study aimed to identify and discuss their immediate prevalence, diagnosis and management at a tertiary care hospital in Pakistan.
-
Methods
- A retrospective study was conducted at a tertiary care hospital in Pakistan between January 2014 and December 2018. All pediatric (<18 years old) patients admitted to the intensive care unit and undergoing continuous electrocardiographic monitoring after surgery for CHD were included in this study. Data pertaining to the incidence, diagnosis, and management of postoperative arrhythmias were collected.
-
Results
- Amongst 812 children who underwent surgery for CHD, 185 (22.8%) developed arrhythmias. Junctional ectopic tachycardia (JET) was the most common arrhythmia, observed in 120 patients (64.9%), followed by complete heart block (CHB) in 33 patients (17.8%). The highest incidence of early postoperative arrhythmia was seen in patients with atrioventricular septal defects (64.3%) and transposition of the great arteries (36.4%). Patients were managed according to the Pediatric Advanced Life Support guidelines. JET resolved successfully within 24 hours in 92% of patients, while 16 (48%) patients with CHB required a permanent pacemaker.
-
Conclusions
- More than one in five pediatric patients suffered from early postoperative arrhythmias in our setting. Further research exploring predictive factors and the development of better management protocols of patients with CHB are essential for reducing the morbidity and mortality associated with postoperative arrhythmia.
-
Keywords: arrhythmias; congenital heart disease; junctional ectopic tachycardia; postoperative complications
INTRODUCTION
Cardiac arrhythmias, which are alterations in heart rate or rhythm, are a well-known postoperative complication in children undergoing cardiac surgery, particularly congenital heart disease (CHD) surgery [1]. Arrhythmias often necessitate an intervention, such as a change in medication, the use of a temporary or permanent pacemaker, or electrical cardioversion/defibrillation [2]. Existing literature suggests an incidence of 7.3%–48% in early post operative period [3-6]. Most of these arrhythmias are transient but can be a cause of substantial morbidity and mortality [7]. Arrhythmias in the postoperative period can be attributed to patient-related risk factors, such as the nature and complexity of CHD itself, and surgery-associated risk factors, such as myocardial incision, sutures placed close to the conduction system, electrolyte disturbances, catecholamine stimulation, cardiopulmonary bypass (CPB)-related inflammation, residual hemodynamic impairment, and arrhythmogenic effects of drugs used commonly during postoperative care [7-9]. While both tachyarrhythmia and bradyarrhythmia may be seen postoperatively, junctional ectopic tachycardia (JET) remains the most common postoperative arrhythmia [10].
A study by Talwar et al. [11] in India found the incidence of postoperative arrhythmias after pediatric cardiac surgery to be 7.5%, with the most common being JET (46.6%). Similarly, a study from Turkey reported an arrhythmia incidence of 8.8%, with 41.2% of cases being JET [6]. However, another study from India by Jain et al. [12] documented an incidence of 14.4%, with complete heart block (CHB) being the most common (36.4%). Meanwhile, though other countries within the region have studied the prevalence of arrhythmias in the early postoperative period after surgery for pediatric CHD, there exists a dearth of data available from Pakistan. Thus, our study aims to describe the distribution of the types of arrhythmias seen in the immediate postoperative period in the pediatric population undergoing surgery for CHD at a tertiary care hospital in Pakistan. In addition, we also discuss our experience in the management of postoperative arrhythmias at our institution.
MATERIALS AND METHODS
Study Setting and Sample
This retrospective study included all pediatric patients who were operated upon for CHD and admitted postoperatively to the pediatric cardiac intensive care unit (PCICU) at the Aga Khan University Hospital, Karachi, between January 2014 and December 2018. The study was reviewed and approved by the Ethics Review Committee of the Aga khan university Hospital prior to data collection. Informed consent was waived as this was a retrospective chart review by the Ethics Review Committee.
Participating children were under the joint care of the critical care consultant, cardiologists, and cardiothoracic surgeons. Patients were put on continuous electrocardiographic (ECG) equipment connected to a central monitoring station. Patients were excluded if they had any preoperative arrhythmia or preexisting heart block, if they had received any anti-arrhythmic therapy before admission to the PCICU, or if they expired within 24 hours postoperatively without experiencing an arrhythmia.
Data Collection
Data were collected on a structured proforma. Variables include demographics (age, sex), anthropometric measures (weight, height), type of heart disease operated upon (congenital, acquired), Risk Adjustment for Congenital Heart Surgery 1 (RACHS-1) score [13], type of surgical procedure, perioperative parameters (CPB time, aortic cross-clamp time), and postoperative data (vasoactive inotropic score [1×dopamine dose {μg/kg/min}, 100×epinephrine dose {μg/kg/min}], duration of mechanical ventilation, PCICU and hospital lengths of stay). Age was categorized as 1 month up to including 1 year (infants), greater than 1 year up to including 6 years (early childhood), greater than 6 years up to including 12 years (late childhood), or greater than 12 years up to including 18 years (adolescence) so as to provide a holistic representation of the spectrum of patients’ ages seen in our setting.
For all patients included, postoperative ECGs were analyzed in accordance with standard clinical practice during their stay in the cardiac intensive care unit. The standard ECG tracings were analyzed independently by cardiologist (SA) and intensivist (AH), and inter-rater reliability was assessed by the calculation of Cohen’s kappa. A kappa value of 0.96 indicated excellent agreement between the two observers.
The presence of arrhythmia was defined as any change in heart rate or rhythm other than sinus either lasting for more than 30 seconds or necessitating an intervention to revert it to sinus rhythm or to control high heart rate. An early postoperative arrhythmia was defined as any such rate or rhythm abnormality documented within the first 24 hours after surgery. All types of arrhythmias were included in this study, including supraventricular tachycardia, reentrant tachycardia, JET, atrial flutter/fibrillation, ventricular tachycardia, ventricular fibrillation, second- and third-degree atrioventricular block, and premature ventricular contractions. For the purpose of this study, frequent premature ventricular beats were considered to be significant if their number exceeded 10 per minute. For each case of arrhythmia, the onset, type, and treatment modality were recorded. Patients were monitored using bedside monitors in the PCICU.
The management team at our institution consists of an intensivist, cardiologist, cardiothoracic surgeon, and PCICU bedside care provider (who provides basic life support and pediatric advanced life support [14] and is a Pediatric Advanced Life Support [PALS]-certified on-call senior resident from the department of pediatrics with good knowledge of ECG patterns, diagnosis, and management of arrhythmias). A focus on a multi-disciplinary team approach to managing the critically ill child is emphasized. Rhythm disturbances, once noticed, were identified by the PCICU bedside care provider, and ECG recordings were taken from either the central recorder or from a 12-lead ECG. The abnormal rhythm and rate were then discussed with the intensivist, who would then consult with the cardiologist and cardiothoracic surgeon on the management team to arrive at a conclusive diagnosis and determine the need for intervention. For all patients, levels of serum electrolytes (sodium, potassium, and ionized calcium) and lactate were measured as needed at hourly intervals from the time of PCICU admission. The decision to treat arrhythmias was made by the management team on a case-by-case basis according to the PALS guideline.
Data Analysis
Data were analyzed using the IBM SPSS ver. 21.0 (IBM Corp., Armonk, NY, USA). The normality of continuous data was assessed using the Shapiro-Wilk test. Continuous variables were expressed as mean±standard deviation values, and categorical variables were expressed as frequencies and percentages. Univariate and multivariate analysis logistic regression was performed with postoperative arrhythmia as the outcome. For the purpose of regression, CBP and aortic cross-clamp times were dichotomized using cut-offs of greater than 120 minutes and greater than 60 minutes (chosen by consensus of cardiac surgeons and anesthesiologists at the Aga Khan University Hospital), respectively, while the RACHS-1 category was dichotomized as less than category 3 or as category 3 or above, respectively. Variables with a P-value of less than 0.25 in the univariate regression were included in the adjusted multivariable model. A P-value of less than 0.05 was considered to be statistically significant for all analyses.
RESULTS
Preoperative, Intraoperative, and Postoperative Characteristics
A total of 812 pediatric patients underwent open cardiac surgeries for CHD between January 2014 and December 2018. Of these, 518 children (63.8%) were male, and the majority were aged between 1 and 6 years (54.4%) or 6 and 12 years (30.9%). The most common diagnoses were ventricular septal defects (VSDs; 48.5%), tetralogy of Fallot’s (TOF; 33.5%), and atrial septal defect (7%). Intraoperatively, the average CPB time and aortic cross-clamp time were 140.4±70.2 minutes and 55.6±27.4 minutes, respectively. Postoperatively, the average duration of ventilation was 32.4±30.2 hours and the average PCICU length of stay was 4.8±2.4 days. Early postoperative arrhythmias occurred in 185 patients (22.8%). Patient preoperative, intraoperative, and postoperative characteristics are described in Table 1. The prevalence rates of arrhythmias associated with different congenital heart defects among our patient cohort are presented in Table 2.
Incidence and Distribution of Arrhythmias
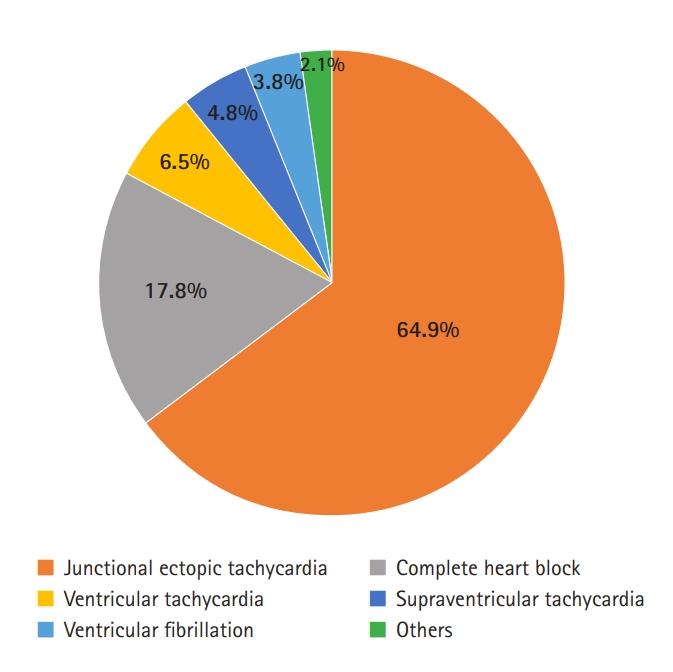
Amongst the 185 patients with arrhythmias in the early postoperative period, JET was the most frequently observed rhythm abnormality (n=120, 64.9%), followed by CHB in 33 patients (17.8%). The distribution of arrhythmias is shown in Figure 1. With respect to the type of CHD (Table 2), the greatest incidence of early postoperative arrhythmia was seen in patients with atrioventricular septal defects (AVSDs; 64.3%), transposition of the great arteries (36.4%), anomalous left coronary artery from the pulmonary artery (33.3%), and TOF (19.1%).
Risk Factors and Associated Analysis
During multivariable analysis, a CPB time of greater than 120 minutes (odds ratio [OR], 2.32; 95% confidence interval [CI], 1.82–4.14), total duration of surgery (OR, 4.33; 95% CI, 2.81–7.14), serum lactate (OR, 3.43; 95% CI, 1.65–5.09), vasoactive inotropic score (OR, 2.51; 95% CI, 1.21–3.72), and RACHS-1 category of greater than 3 (OR, 2.23; 95% CI, 1.83–4.08) were found to be independent risk factors for the development of postoperative arrhythmias (Table 3).
Management and Outcomes
While none of the early postoperative CHB events were hemodynamically significant, temporary cardiac pacing was required in all patients with CHB. Seventeen patients (52%) recovered within 10 days of dexamethasone therapy, while the remaining 16 (48%) required a permanent pacemaker since the CHB persisted for more than 10 days.
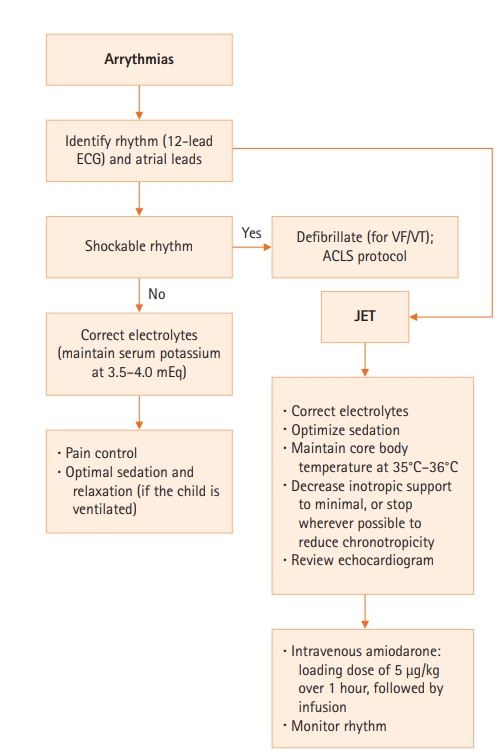
Of the 120 patients with JET, 25 (21%) responded to conventional measures, including temperature control by surface cooling, pain control, withdrawal of inotropes, and electrolyte correction (Figure 2). Two patients reverted to sinus rhythm once they recovered from low cardiac output syndrome; the rest were converted to normal sinus rhythm after receiving an amiodarone loading dose of 5 μg/kg/min bolus, followed by 10 μg/kg/min by intravenous infusion in cases that were unresponsive to other treatment modalities. JET resolved successfully within 24 hours in 92% of patients.
Of the 185 patients with early postoperative arrhythmias, 145 (78%) converted to sinus rhythm within the first 24 hours. Following AVSD repair, two patients died of low cardiac output syndrome secondary to refractory JET. Five patients with TOF and one patient with VSD also expired due to arrhythmia-induced low cardiac output syndrome. One patient died later on during the course of hospitalization, although the cause of death could not be attributed directly to an arrhythmia. These eight patients (4.3%) constituted the only deaths in our cohort with postoperative arrhythmias. However, a total of 18 patients (2.9%) amongst those without postoperative arrhythmias died.
If the observed rate and rhythm disturbances were found to be benign (infrequent premature ventricular contractions/ventricular bigeminy/atrial premature contractions/short run of ventricular tachycardia), patients were managed with a “watchful waiting” policy involving routine de-escalation/withdrawal of exogenous catecholamines and routine measures to control hyperthermia. Most of the rhythm disturbances could eventually be treated using the PALS guidelines.
DISCUSSION
Postoperative arrhythmias are a well-known complication in children, particularly after surgery for CHD. This study explored the incidence, diagnosis, and management of common rhythm disturbances in the pediatric population following surgery for CHD repair over a 5-year period at a tertiary care hospital in Pakistan. In addition, we also discuss our experience in the management of postoperative arrhythmias at our institution.
Postoperative arrythmias can lead to higher morbidity and mortality in children [5,15]. The incidence of postoperative arrhythmias in children has been reported to be as high as 48% despite recent improvements [6,16]. Our study shows the prevalence of hemodynamically significant arrhythmias to be 22.8%. This is higher than the rate observed in studies from other countries in the region, such as India and Turkey [6,8,11,16]. However, other recent studies have offered results similar to ours [3], including a study from Bangladesh, which reported an incidence of 31% [17]. The relatively high incidence of arrhythmias in our study may be related to surgical factors, especially the myocardial protection techniques used in the operating theatre. The mean CPB time was 140 minutes in our study, which is higher compared to in previous studies [3], which may be a contributing factor. This highlights a challenge in low-resource settings, such as those in Pakistan, where optimal myocardial protection may not be achievable and there is a shortage of specialized perfusionists. Lastly, however, the mean length of PCICU stay was acceptable at approximately 5 days, although slightly longer than that reported in the literature. A study from the United Kingdom reported the median PCICU length of stay after pediatric cardiac surgery to be around 3 days [18], while a study from Poland reported a median of 2 days [19].
JET was found to be the most frequently occurring arrhythmia amongst our study patients. This finding is corroborated by previous studies from India and Turkey, with JET constituting up to 60% of recorded arrhythmias [6,8,11]. The mechanism of JET is believed to be due to direct trauma to the atrioventricular node and bundle of His, although JET also occurs in patients in whom there is no operation near the atrioventricular node. Literature suggests that the type of CHD and the surgical correction (e.g., VSD, TOF, AVSD repair) can be major causes of the development of postoperative JET [20,21]. In the current study, 25 patients (21%) responded to conventional measures, whereas the rest required additional therapy in the form of amiodarone infusion. JET resolved successfully in 92% of all cases. In the study by Abdelaziz and Deraz [22], JET was successfully resolved in 86.5% of patients, with 57% responding to conventional measures and the remaining 43% controlled by amiodarone infusion in addition to conventional measures.
The high incidence of arrhythmias in our study may be related to surgical factors, especially the myocardial protection techniques used in the operating theatre. Most of our patients with arrhythmias had a prolonged CBP time lasting more than 100 minutes on average, an inotropic score of more than 20 points, and an elevated level postoperatively. The relatively high incidence in some, but not all reports, may be related to a variability of arrhythmias chosen for analysis.
CHB accounted for 33% of the arrhythmias in our patient cohort. Atrioventricular block is common in surgeries involving manipulation around the conducting system. CHB following surgical repair may be transient or permanent. In the current study, approximately half of our CHB cases recovered within 10 days on steroids, with the remaining patients requiring permanent pacemakers. Since the numbers are more or less equal, further studies are required to establish the effectiveness of steroids and optimal timing and indications for pacemaker placement in patients who develop CHB.
This was a single-center study, and its findings may not be generalizable to other centers in Pakistan or elsewhere in the world. Moreover, we did not record or report exact times by which arrhythmias reverted to normal sinus rhythm in patients. In conclusion, more than one in five pediatric patients suffered from early postoperative arrhythmias in our setting. Further research exploring predictive factors and the development of better management protocols of patients with CHB are essential for reducing the rates of morbidity and mortality associated with postoperative arrhythmia in Pakistan.
KEY MESSAGE
▪ We report a 22.8% rate of postoperative arrhythmias in patients who underwent surgery for congenital heart disease.
▪ Junctional ectopic tachycardia was the most common arrhythmia (65%), followed by complete heart block (17.8%).
▪ Postoperative arrhythmia was seen most commonly in patients with atrioventricular septal defects (64.3%) and transposition of the great arteries (36.4%).
NOTES
-
CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
Conceptualization: SI, SS, AUH. Data curation: SI, SS, ARK, FM. Formal analysis: SI, RSM. Methodology: SI, SS, MKYM. Project administration: SI, SS, AUH. Writing–original draft: SI, AAL, RSM, MKYM, ARK, FM, AUH. Writing–review & editing: SI, SS, AAL, RSM.
Figure 1.Types of early postoperative arrhythmias.
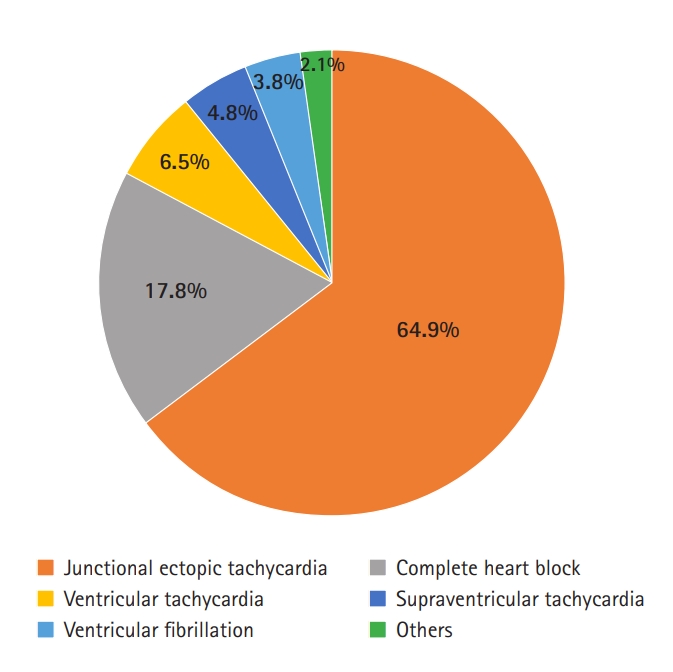
Figure 2.Algorithm for the management of postoperative tachyarrhythmias in a Pakistani pediatric population after surgery for congenital heart disease. ECG: electrocardiography; VF: ventricular fibrillation; VT: ventricular tachycardia; ACLS: advanced cardiovascular life support; JET: junctional ectopic tachycardia.
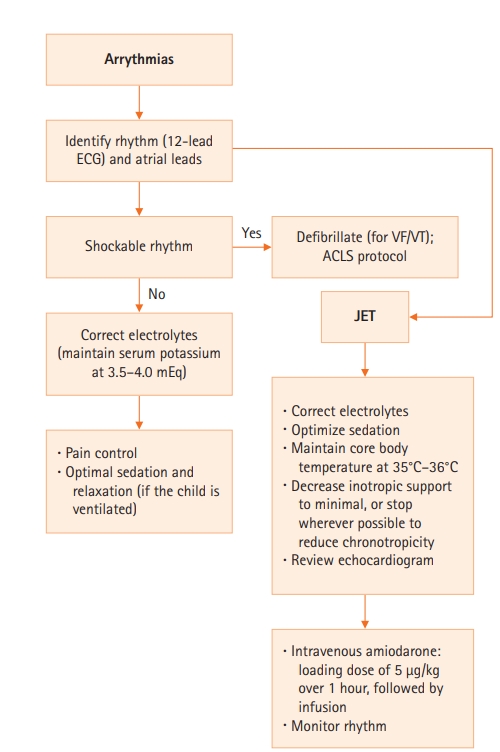
Table 1.Preoperative, intraoperative, and postoperative characteristics
|
Variable |
Value (n=812) |
|
Age group |
|
|
1 mo to ≤1 yr (infant) |
46 (5.7) |
|
>1 to ≤6 yr (early childhood) |
442 (54.4) |
|
>6 to ≤12 yr (late childhood) |
251 (30.9) |
|
>12 to ≤18 yr (adolescence) |
73 (9.0) |
|
Sex |
|
|
Male |
518 (63.8) |
|
Female |
294 (36.2) |
|
Weight (kg) |
12.7±13.5 |
|
Length/height (cm) |
78.2±15.4 |
|
Diagnosis |
|
|
Ventricular septal defect |
394 (48.5) |
|
Tetralogy of Fallot |
272 (33.5) |
|
Atrial septal defect |
57 (7.0) |
|
Atrioventricular septal defect |
14 (1.7) |
|
Transposition of the great arteries |
11 (1.4) |
|
Coarctation of aorta/interrupted aortic arch |
18 (2.2) |
|
Anomalous left coronary artery from the pulmonary artery |
3 (0.3) |
|
Miscellaneous (single-ventricle physiology) |
43 (5.3) |
|
Cardiopulmonary bypass time (min) |
140.4±70.2 |
|
Aortic cross-clamp time (min) |
55.6±27.4 |
|
Duration of mechanical ventilation (hr) |
32.4±30.2 |
|
Vasoactive inotropic score |
18.5±12.2 |
|
Temperature during surgery (°C) |
30.8±2.8 |
|
Duration of surgery (hr) |
5.5±1.2 |
|
Early postoperative arrhythmias |
185 (22.8) |
|
PCICU stay (day) |
4.8±2.4 |
Table 2.Frequency of different types of arrhythmias across different CHDa
|
Type of arrhythmias |
TOF (n=272) |
VSD (n=394) |
ASD (n=57) |
AVSD (n=14) |
TGA (n=11) |
COA/IAA (n=18) |
ALCAPA (n=3) |
|
Overall |
52 (19.1) |
26 (6.6) |
4 (7.0) |
9 (64.3) |
4 (36.4) |
3 (16.7) |
1 (33.3) |
|
JET |
37 (13.6) |
26 (6.6) |
2 (3.5) |
3 (21.4) |
4 (36.4) |
3 (16.7) |
0 |
|
VT |
11 (4.0) |
0 |
0 |
0 |
0 |
0 |
1 (33.3) |
|
VF |
0 |
0 |
0 |
0 |
0 |
0 |
0 |
|
CHB |
2 (0.7) |
0 |
0 |
6 (42.9) |
0 |
0 |
0 |
|
MAT |
1 (0.4) |
0 |
0 |
0 |
0 |
0 |
0 |
|
EAT |
1 (0.4) |
0 |
0 |
0 |
0 |
0 |
0 |
|
SVT |
0 |
0 |
2 (3.5) |
0 |
0 |
0 |
0 |
Table 3.Risk factors for arrhythmia in the study identified on multivariable logistic regression analysis
|
Variable |
Adjusted odds ratio (95% CI) |
P-value |
|
Age (yr) |
3.35 (2.29–5.64) |
0.492 |
|
CBP time >120 min |
2.32 (1.82–4.14) |
<0.005 |
|
ACC time >60 min |
1.97 (0.68–2.66) |
0.432 |
|
Surgery duration (hr) |
4.33 (2.81–7.14) |
<0.001 |
|
Duration of mechanical ventilation (hr) |
1.34 (0.39–1.76) |
0.863 |
|
RACHS-1 category ≥3 |
2.23 (1.83–4.08) |
0.046 |
|
Serum lactate (mmol/L) |
3.43 (1.65–5.09) |
0.003 |
|
Heart rate (beats/min) |
1.89 (1.05–3.94) |
0.120 |
|
VIS |
2.51 (1.21–3.72) |
<0.001 |
References
- 1. Romer AJ, Tabbutt S, Etheridge SP, Fischbach P, Ghanayem NS, Reddy VM, et al. Atrioventricular block after congenital heart surgery: analysis from the Pediatric Cardiac Critical Care Consortium. J Thorac Cardiovasc Surg 2019;157:1168-77.e2.ArticlePubMed
- 2. Delaney JW, Moltedo JM, Dziura JD, Kopf GS, Snyder CS. Early postoperative arrhythmias after pediatric cardiac surgery. J Thorac Cardiovasc Surg 2006;131:1296-300.ArticlePubMed
- 3. Pfammatter JP, Bachmann DC, Wagner BP, Pavlovic M, Berdat P, Carrel T, et al. Early postoperative arrhythmias after open-heart procedures in children with congenital heart disease. Pediatr Crit Care Med 2001;2:217-22.ArticlePubMed
- 4. Hoffman TM, Wernovsky G, Wieand TS, Cohen MI, Jennings AC, Vetter VL, et al. The incidence of arrhythmias in a pediatric cardiac intensive care unit. Pediatr Cardiol 2002;23:598-604.ArticlePubMed
- 5. Choi HJ, Kim YH, Cho JY, Hyun MC, Lee SB, Kim KT. Early postoperative arrhythmias after open heart surgery of pediatric congenital heart disease. Korean J Pediatr 2010;53:532-7.Article
- 6. Yildirim SV, Tokel K, Saygili B, Varan B. The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients. Turk J Pediatr 2008;50:549-53.PubMed
- 7. Kabbani MS, Al Taweel H, Kabbani N, Al Ghamdi S. Critical arrhythmia in postoperative cardiac children: recognition and management. Avicenna J Med 2017;7:88-95.ArticlePubMedPMC
- 8. Sahu MK, Das A, Siddharth B, Talwar S, Singh SP, Abraham A, et al. Arrhythmias in children in early postoperative period after cardiac surgery. World J Pediatr Congenit Heart Surg 2018;9:38-46.ArticlePubMed
- 9. Anselmi A, Abbate A, Girola F, Nasso G, Biondi-Zoccai GG, Possati G, et al. Myocardial ischemia, stunning, inflammation, and apoptosis during cardiac surgery: a review of evidence. Eur J Cardiothorac Surg 2004;25:304-11.ArticlePubMed
- 10. Cools E, Missant C. Junctional ectopic tachycardia after congenital heart surgery. Acta Anaesthesiol Belg 2014;65:1-8.PubMed
- 11. Talwar S, Patel K, Juneja R, Choudhary SK, Airan B. Early postoperative arrhythmias after pediatric cardiac surgery. Asian Cardiovasc Thorac Ann 2015;23:795-801.ArticlePubMed
- 12. Jain A, Alam S, Viralam SK, Sharique T, Kapoor S. Incidence, risk factors, and outcome of cardiac arrhythmia postcardiac surgery in children. Heart Views 2019;20:47-52.ArticlePubMedPMC
- 13. Jenkins KJ, Gauvreau K, Newburger JW, Spray TL, Moller JH, Iezzoni LI. Consensus-based method for risk adjustment for surgery for congenital heart disease. J Thorac Cardiovasc Surg 2002;123:110-8.ArticlePubMed
- 14. de Caen AR, Berg MD, Chameides L, Gooden CK, Hickey RW, Scott HF, et al. Part 12: pediatric advanced life support: 2015 American Heart Association Guidelines update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation 2015;132(18 Suppl 2):S526-42.PubMedPMC
- 15. Lan YT, Lee JC, Wetzel G. Postoperative arrhythmia. Curr Opin Cardiol 2003;18:73-8.ArticlePubMed
- 16. Hoffman TM, Bush DM, Wernovsky G, Cohen MI, Wieand TS, Gaynor JW, et al. Postoperative junctional ectopic tachycardia in children: incidence, risk factors, and treatment. Ann Thorac Surg 2002;74:1607-11.ArticlePubMed
- 17. Hoque KZ, Sultana AT, Mia M, Chowdhury MG, Hossein M. Early postoperative arrhythmias after paediatric cardiac surgery. Delta Med Coll J 2018;6:22-8.Article
- 18. Brown KL, Ridout DA, Goldman AP, Hoskote A, Penny DJ. Risk factors for long intensive care unit stay after cardiopulmonary bypass in children. Crit Care Med 2003;31:28-33.ArticlePubMed
- 19. Pagowska-Klimek I, Pychynska-Pokorska M, Krajewski W, Moll JJ. Predictors of long intensive care unit stay following cardiac surgery in children. Eur J Cardiothorac Surg 2011;40:179-84.ArticlePubMed
- 20. Paul T, Ziemer G, Luhmer L, Bertram H, Hecker H, Kallfelz HC. Early and late atrial dysrhythmias after modified Fontan operation. Pediatr Med Chir 1998;20:9-11.PubMed
- 21. Dodge-Khatami A, Miller OI, Anderson RH, Goldman AP, Gil-Jaurena JM, Elliott MJ, et al. Surgical substrates of postoperative junctional ectopic tachycardia in congenital heart defects. J Thorac Cardiovasc Surg 2002;123:624-30.ArticlePubMed
- 22. Abdelaziz O, Deraz S. Anticipation and management of junctional ectopic tachycardia in postoperative cardiac surgery: single center experience with high incidence. Ann Pediatr Cardiol 2014;7:19-24.ArticlePubMedPMC
Citations
Citations to this article as recorded by

- Prevalence and risk factors analysis of early postoperative arrhythmia after congenital heart surgery in pediatric patients
Ketut Putu Yasa, Arinda Agung Katritama, I. Komang Adhi Parama Harta, I. Wayan Sudarma
Journal of Arrhythmia.2024; 40(2): 356. CrossRef - Improvements in Accuracy and Confidence in Rhythm Identification After Cardiac Surgery Using the AtriAmp Signals
Diane H. Brown, Xiao Zhang, Awni M. Al-Subu, Nicholas H. Von Bergen
Journal of Intensive Care Medicine.2023; 38(9): 809. CrossRef
 , Saleem Akhtar1
, Saleem Akhtar1 , Asma Akbar Ladak2
, Asma Akbar Ladak2 , Russell Seth Martins2
, Russell Seth Martins2 , Muhammad Kamran Younis Memon3
, Muhammad Kamran Younis Memon3 , Alisha Raza Kazmi2
, Alisha Raza Kazmi2 , Fatima Mahmood2
, Fatima Mahmood2 , Anwar ul Haque3
, Anwar ul Haque3






 KSCCM
KSCCM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite